Apple Watch Sleep Apnea Detection: What It Can and Can’t Do
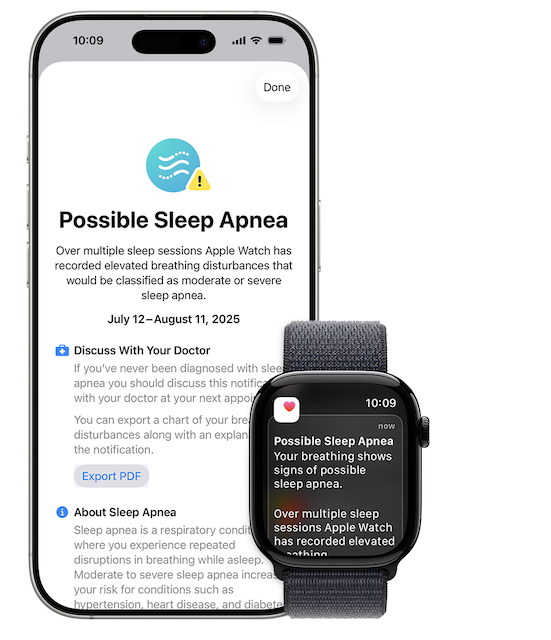
When Apple announced that the Series 9 and Series 10 would include FDA-cleared sleep apnea detection, my first reaction was something between excitement and wistfulness. The technology that might have flagged my condition years earlier now fits on anyone’s wrist.
I spent years with undiagnosed obstructive sleep apnea before I finally got tested and diagnosed. The migraines, the exhaustion, the brain fog I’d been normalising as just the way adult life felt: all of it had a cause that a proper sleep assessment would have identified much earlier. I didn’t get that assessment because nobody suggested I needed one. After all, the symptoms are easy to attribute to other things, and there was no particular moment of alarm that pushed me toward a doctor.
The Apple Watch feature is interesting to me specifically because it creates that moment of alarm for people who might otherwise never have one.
What the Watch Actually Does
The sleep apnea detection doesn’t work the way a medical sleep study works. It doesn’t measure airflow, oxygen saturation, or brain activity. What it does is use the watch’s accelerometer to detect tiny wrist movements that correlate with breathing disturbances during sleep. Over thirty days, if it detects a consistent pattern of elevated disturbances across multiple nights, it alerts you.
Apple received FDA 510k clearance for this feature in September 2024, which classifies it as an over-the-counter screening device rather than a diagnostic tool. That distinction matters and I’ll come back to it. The clearance means it’s met regulatory standards for consumer use as a screening aid, not that it can tell you whether you have sleep apnea in the clinical sense.
The accuracy figure that’s been reported from Apple’s validation study is around 66% sensitivity for moderate to severe sleep apnea. That means roughly two in three people with moderate to severe OSA will receive an alert. The other third won’t, either because their particular presentation doesn’t produce the wrist movement patterns the algorithm is looking for, or because their apnea is mild enough to fall below the detection threshold.
For a device worn on your wrist that requires zero additional equipment or effort, that’s a meaningful capability. For comparison, the majority of the estimated 30 million Americans with sleep apnea have never been diagnosed at all, not because the tools don’t exist but because nothing prompted them to use those tools. A 66% chance of catching moderate to severe OSA through something people are already wearing every day is genuinely significant public health progress.
The Important Limitation
The alert is the beginning of the process, not the end of it.
This is where I want to be direct, because I’ve seen the Apple Watch sleep apnea feature described in ways that suggest getting an alert means getting a diagnosis. It doesn’t. What it means is that you’ve been flagged as potentially having moderate to severe sleep apnea and should get properly tested.
A proper test matters because it’s what gets you treatment. You cannot get a CPAP prescription based on a watch alert. You cannot submit to insurance based on a watch alert. You need a clinically validated sleep study, either a home sleep test or an in-lab polysomnography, that measures actual airflow, oxygen levels and sleep architecture rather than wrist movements. That assessment is what confirms whether you have sleep apnea, how severe it is, and what treatment is appropriate.
The at-home sleep test route has become much more accessible and affordable than it used to be. I’ve reviewed the WatchPAT One in detail: it’s FDA-cleared for diagnosis, measures multiple physiological channels, and produces a report that a sleep physician can use to prescribe treatment. For most people who receive an Apple Watch alert, this is the logical next step rather than booking an in-lab study. If the home test comes back unclear or if there are complicating factors, the in-lab study remains the gold standard.
The watch also won’t reliably detect mild sleep apnea or central sleep apnea, both of which require the more comprehensive measurement that proper sleep testing provides. If you have symptoms that concern you but don’t receive an alert, that’s not a clean bill of health.
What It Means for People Who Haven’t Been Diagnosed
The sleep apnea population is thought to be vastly underdiagnosed. Research consistently shows that the majority of people with moderate to severe OSA remain unaware of it. They attribute the symptoms to other things, they don’t have partners who’ve noticed, or they simply haven’t crossed the threshold of concern that sends someone to a doctor.
The Apple Watch feature changes the dynamic slightly. It means that for hundreds of millions of people who already own a compatible device, the watch is now quietly monitoring for signs of a serious condition every time they sleep. That passive screening, even at 66% sensitivity, represents a meaningful shift in how likely undiagnosed sleep apnea is to be caught.
I think about the version of me from a decade ago. I owned a smartwatch. If it had flagged something, if there had been a notification on my phone one morning saying the watch had detected consistent breathing disturbances and recommending I speak to a doctor, I would have acted on it. The problem wasn’t that I lacked access to testing. It was that I had no reason to seek it out.
That’s what this technology addresses, and why I think the headline sensitivity figure of 66% slightly undersells the value. The comparison isn’t between Apple Watch and a diagnostic sleep study. It’s between Apple Watch and nothing, which is what most undiagnosed people currently have.
If You Already Have a Diagnosis
The feature is designed for people without a prior sleep apnea diagnosis, and Apple is explicit that it’s not intended as a monitoring tool for people already in treatment. If you’re already on CPAP therapy, the watch’s breathing disturbance metric isn’t a meaningful measure of how well your therapy is controlling your apnea. Your machine’s own data, accessible through apps like MyAir, gives you much more relevant information about therapy effectiveness than wrist accelerometry can.
For monitoring therapy, the numbers that matter are the ones your CPAP is recording directly: event frequency, leak rate, and pressure data. I’ve written about how to interpret your CPAP data separately for anyone who wants to go deeper on that.
The Broader Picture
The Apple Watch feature is one part of a broader shift toward consumer technology that can flag serious health conditions that previously required clinical intervention to detect. It’s not a replacement for proper medical assessment, and Apple is appropriately clear about that in how they’ve positioned it. But as a first-line screening tool that meets people where they already are, wearing a device they already own, it represents genuine progress.
If you have a compatible watch and haven’t turned the feature on, it’s worth enabling through the Health app under Respiratory. It requires at least ten nights of sleep data collected over thirty days and at least four hours of wear per night, so consistency matters. If you get an alert, take it seriously and get properly tested rather than either panicking or dismissing it.
And if you don’t get an alert but still have the symptoms I described experiencing for years, persistent morning headaches, waking unrefreshed, a heaviness through the day that doesn’t match how long you slept, the absence of an alert doesn’t mean the absence of a problem. The watch catches what it can see. A proper sleep test catches everything.
⚠️ MEDICAL DISCLAIMER This blog provides general information only and is not a substitute for professional medical advice, diagnosis, or treatment. Sleep apnea is a serious condition, and CPAP equipment should be used under proper medical supervision. Always consult your doctor or sleep specialist before starting, stopping, or changing any therapy. I share personal experiences as a CPAP user, not as a medical professional. Individual results vary. For medical guidance, please consult a qualified clinician or the American Academy of Sleep Medicine (aasm.org).





