Can a Deviated Septum Cause Sleep Apnea?
I had my septoplasty years before anyone ever mentioned sleep apnea to me. Looking back, the two were almost certainly connected the whole time. I just didn’t know it yet.

My septum had been off since I was a kid. Most people say they are a result of a sports injury, but for me, I think I was born with it.
I had chronic congestion growing up, regular sinus infections, and I always resorted to mouth breathing after basic exercise. When a surgeon finally straightened it out, the difference was remarkable. I could breathe freely through my nose for the first time in years. Exercise felt easier. I slept better for a while.
Then, about 10 years later, I was diagnosed with severe obstructive sleep apnea. Turns out I’d had it for a while. The septoplasty had helped, but it hadn’t fixed the underlying problem because it couldn’t — the two conditions are related, but they’re not the same thing.
If you’re dealing with both a deviated septum and sleep apnea, or you’re trying to figure out whether one is causing the other, here’s what I wish someone had explained to me clearly before I went through all of it.
What a Deviated Septum Actually Is
The septum is the wall of cartilage and bone running down the middle of your nose, dividing it into two passages. In theory, it sits straight and even. In practice, most people’s septa are at least a little off centre. For most people, that doesn’t matter much. But when the deviation is significant enough to obstruct airflow through one side, you start to notice it.
Common signs include congestion that always seems worse on one side, frequent nosebleeds, recurrent sinus infections, and noisy or laboured breathing at night. Some people notice they can only really breathe freely through one nostril at a time. Others just feel perpetually blocked without knowing why.
A deviated septum happens in two main ways: you’re either born with one, or you develop it from an injury. Childhood and teenage years are a common time for the injury type — a knock to the nose during sport, a fall, anything that shifts the cartilage. The deviation often becomes more noticeable over time as the nose finishes developing.
The Sleep Apnea Connection
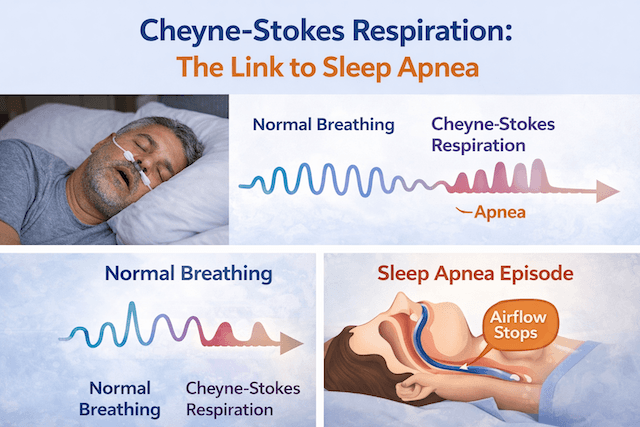
Sleep apnea is what happens when your airway repeatedly collapses during sleep, cutting off your breathing in short bursts throughout the night. Your brain kicks you out of deep sleep to restart breathing, and this cycle repeats so many times that you never get the restorative rest you need. The obstruction happens in the throat, not the nose — at the level of the soft palate, the tongue, or the back of the pharynx.
So a deviated septum doesn’t directly cause sleep apnea. That’s worth being clear about upfront. But it absolutely makes sleep apnea worse, and here’s why that matters.
When your nasal passage is obstructed, your body compensates by breathing through your mouth while you sleep. Mouth breathing changes the dynamics of your upper airway. The tongue and jaw shift position, the throat becomes the primary breathing channel, and the chances of airway collapse go up significantly. Nasal breathing provides a kind of natural resistance that helps keep the airway stable. Lose that, and you lose the protection too.
The result is that someone with a moderate predisposition to sleep apnea might develop a much more severe case because their deviated septum is constantly pushing them towards mouth breathing at night. Or they might find that even mild sleep apnea comes with much heavier symptoms than you’d expect — the congestion, the poor sleep quality, the daytime fog — because the nasal obstruction is compounding everything.
A large study following over a million people found that those with septal deviation had significantly higher rates of obstructive sleep apnea than those without. That’s not proof of direct causation, but it’s a strong signal that the two conditions are feeding each other.
My Experience
When I was finally diagnosed with sleep apnea, one of my first thoughts was, “But I had my septum fixed.” And technically, I had. My nasal passages were much clearer than they’d been before surgery. But the OSA was still there, still severe in severity, still doing damage every night.
My sleep specialist explained it well. The septoplasty had probably stopped things from getting worse. I likely already had sleep apnea before the surgery, and the nasal obstruction was making the symptoms heavier than they needed to be. Fixing the nose improved my breathing and probably knocked the severity down a notch. But the throat anatomy that was actually causing the apneas — the way my airway collapsed when I relaxed — that was still there waiting to be dealt with.
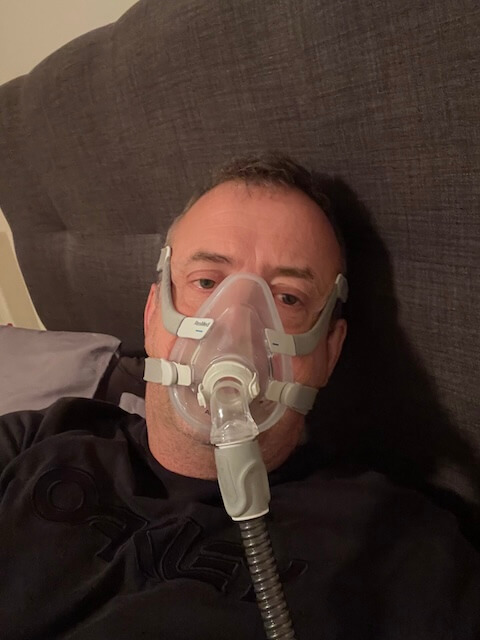
My first night on CPAP was genuinely rough. The mask felt strange, the pressure felt strange, and I wasn’t convinced any of it was going to help. Within a week, the difference in how I felt during the day was undeniable. Within a month, I couldn’t imagine going back. Clear nasal passages definitely made getting used to CPAP easier — I suspect it would have been harder to adapt if I’d still been working with a heavily obstructed nose.
Does Fixing the Septum Help with Sleep Apnea?
Yes and no, and the honest answer depends on what you’re hoping to fix.
The research on septoplasty and sleep apnea shows a consistent split between objective and subjective outcomes. Objectively, fixing the septum rarely cures sleep apnea on its own or brings the number of apnea events down dramatically. Subjectively, most patients feel meaningfully better — they sleep better, feel less sleepy during the day, and often snore less. Septoplasty combined with turbinate reduction (addressing the swollen tissue alongside the septum itself) tends to produce the best results.
For people with mild sleep apnea in particular, nasal surgery can sometimes make a real dent. If the nasal obstruction has been a major driver of airway instability, removing it can shift things enough to matter. For moderate or severe sleep apnea, you’re unlikely to reach a point where you no longer need CPAP or another primary treatment — but you may find those treatments become much easier to use.
That’s arguably one of the most practical reasons to address a deviated septum if you have sleep apnea: CPAP therapy is significantly harder to tolerate when your nose is blocked. Nasal masks and nasal pillow masks become almost unusable, and even with a full face mask you’re fighting additional resistance all night. Clearing the nasal airway doesn’t replace CPAP, but it makes CPAP work better.
What Treatment Actually Looks Like
If you have both conditions, you’re likely looking at a combined approach rather than one fix solving everything.
For the deviated septum, the options run from conservative to surgical. Nasal steroid sprays can reduce inflammation and improve airflow without doing anything permanent. Decongestants help in the short term, though they’re not great for regular use. Nasal strips across the bridge of the nose can make a genuine difference at night for some people — worth trying before anything more involved. When symptoms are severe enough to affect daily life, septoplasty is the definitive solution. It’s a routine outpatient procedure; recovery takes a couple of weeks, and for most people, the results are significant and lasting.
For sleep apnea, CPAP remains the most effective treatment for moderate to severe cases regardless of what’s happening with your nose. If you’re newly diagnosed and worried that nasal obstruction will make CPAP impossible to tolerate, it’s worth discussing with your doctor whether to address the nose first or at the same time. The right CPAP mask matters too — if nasal breathing is difficult, a full face mask that covers both nose and mouth gives you more flexibility.
For milder sleep apnea, a sleep apnea mouth guard is worth considering as an alternative to CPAP. These work by repositioning the jaw forward to keep the airway open, and they function independently of nasal breathing, which makes them a practical option if you’re dealing with ongoing nasal issues.
Lifestyle factors also genuinely matter. Excess weight is one of the strongest contributors to sleep apnea severity, and even modest weight loss can reduce the pressure on your airway. Sleeping on your side rather than your back helps most people with OSA, and it’s worth trying before assuming you need anything more complicated.
When to See a Doctor
If you’re snoring heavily, waking up feeling unrefreshed, or your partner has noticed you stopping breathing in the night, get a sleep apnea test. Home sleep tests have become genuinely accessible and affordable, and the sooner you know what you’re dealing with, the sooner you can do something about it. Untreated sleep apnea carries real long-term risks — cardiovascular, metabolic, cognitive — and it tends not to improve on its own.
If you have chronic congestion, one-sided blockage, or recurring sinus infections, mention them. An ENT can assess your nasal anatomy quickly with a simple examination. It’s worth evaluating both conditions together rather than treating them in isolation, because treatment decisions affect each other.
The Bottom Line
A deviated septum doesn’t cause sleep apnea in the direct sense, but it can make it significantly worse and harder to treat. If you have both, addressing the nasal obstruction is worth doing — not because it will cure your sleep apnea, but because it removes one of the things that’s been driving it and makes every other treatment easier to stick with.
I wish I’d known all of this before I had my septoplasty, not because I’d have made a different decision (the surgery was absolutely the right call for me), but because I’d have been watching for sleep apnea sooner rather than assuming the nose surgery had sorted everything out.
If any of this sounds familiar, look into it. The combination of a clear nasal airway and effective sleep apnea treatment genuinely changes how you feel day to day. I know because I’m living on the other side of it.
If you found this useful, my sleep apnea diagnosis guide is a good next read, along with my overview of sleep apnea treatment options if you’re trying to figure out where to start.
⚠️ MEDICAL DISCLAIMER This blog provides general information only and is not a substitute for professional medical advice, diagnosis, or treatment. Sleep apnea is a serious condition, and CPAP equipment should be used under proper medical supervision. Always consult your doctor or sleep specialist before starting, stopping, or changing any therapy. I share personal experiences as a CPAP user, not as a medical professional. Individual results vary. For medical guidance, please consult a qualified clinician or the American Academy of Sleep Medicine (aasm.org).