How Does a CPAP Machine Work: Meet my Life Changing Device!

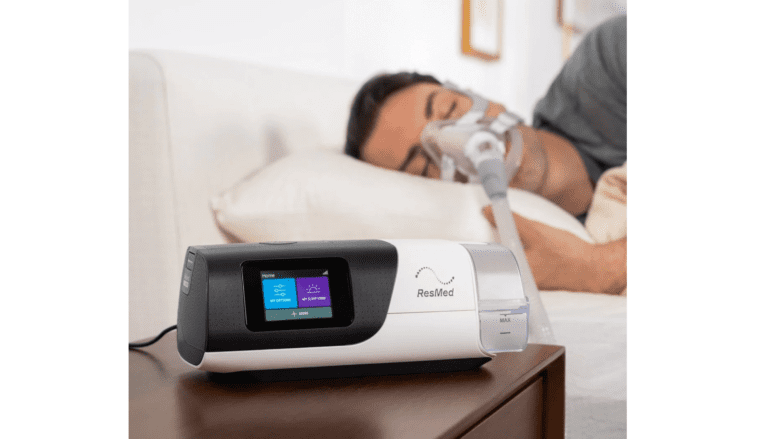
I know this sounds strange, but I’m genuinely grateful for the machine that sits on my nightstand. I’ve been sleeping with it every night for over a decade. It hums quietly beside me while I sleep, connected to a mask on my face, and I’ve reached the point where I feel more comfortable with it on than without it. If you’d told me that in 2014 when I was first handed a prescription and sent home to figure it out, I wouldn’t have believed you.
What changed my relationship with CPAP therapy wasn’t just getting used to it. It was understanding what it actually does. Once I grasped the mechanics, once I understood what was happening inside that box every night and what it was preventing, it stopped feeling like medical equipment I was obliged to use and started feeling like something I actively wanted to use. There’s a difference, and it matters for whether you stick with it.
So let me explain how it works, the way I wish someone had explained it to me at the start.
The Problem It’s Solving
To understand what a CPAP machine does, you have to understand what obstructive sleep apnea actually is. When you fall asleep, the muscles throughout your body relax, including the muscles that keep your upper airway open. In people with OSA, that relaxation goes too far. The soft tissue in the throat collapses inward, the airway closes, and you stop breathing. Your brain detects the oxygen drop, triggers a partial awakening to restore muscle tone, your airway reopens, and you resume breathing. Then you fall back asleep and the whole cycle starts again.
In my case, before I was diagnosed, that was happening 51 times every hour. Once roughly every minute. My blood oxygen was dropping to 78 percent. I had no idea any of it was happening. I just knew I woke up feeling wrecked every morning, had a headache before I’d even opened my eyes, and was grinding through each day in a fog I couldn’t explain.
CPAP solves this through a deceptively simple mechanism. It delivers a continuous stream of pressurised air through a mask while you sleep. That air pressure, maintained constantly throughout the night, prevents the throat tissue from collapsing. Think of it like inflating a balloon slightly. The walls can’t cave in because there’s positive pressure holding them apart. The medical term is a pneumatic splint, which I find satisfying as a description because it captures exactly what it does: it props the airway open with air.
What’s Inside the Machine
The device itself is doing three things simultaneously. It’s filtering the room air coming in, pressurising it to a prescribed level, and in most modern machines humidifying it before it reaches you.
The filtration stage is worth not overlooking. There’s a disposable filter and usually a reusable foam filter that catch dust, allergens, and other airborne particles. I replace the disposable one monthly and wash the foam one weekly. When I’ve let this slip I’ve noticed the difference, the air feels less fresh somehow, which sounds subjective but is consistently real. If you have allergies this matters more than it might seem.
The pressure generation is the core of what the machine does. Inside is a small blower motor that compresses the air to your prescribed level, measured in centimetres of water pressure, written as cmH₂O. The typical range runs from about 4 to 20 cmH₂O. I started at 8 when I was first diagnosed, and after a few months of reviewing my data my sleep specialist increased it to 10, which is where it’s been ever since. Finding the right pressure isn’t always immediate and it’s worth treating it as an ongoing calibration rather than a one-time setting.
The humidifier, which on my ResMed AirSense 10 is integrated into the machine, adds moisture to the pressurised air before it travels through the hose to the mask. This is not optional in any meaningful sense. Breathing dry pressurised air through a mask all night dries out your nose, your throat, and your mouth in ways that range from uncomfortable to genuinely painful. I run my humidifier at level 3 in summer when the air conditioning is on and bump it to level 5 in winter when the central heating dries everything out. It took a bit of trial and error to find the right settings for my environment but it made an enormous difference once I got it right.
The Hose and the Rainout Problem
The hose connects the machine to the mask and it’s where one of the more unpleasant early CPAP experiences can happen: rainout. Rainout is when the warm humid air from the machine cools down as it travels through the hose, condenses into water, and then travels the rest of the way to your face. Waking up at three in the morning with water droplets hitting you from your own CPAP hose is startling in a way that stays with you.
Heated tubing solves this. The hose has a heating element that keeps the air temperature consistent along its entire length, so the moisture stays as vapour rather than condensing. My ResMed has this as a built-in option and I use it every night. If rainout has been a problem for you and you’re not using heated tubing, that’s the first thing to try. I wrote about this in more detail in my rainout guide if you need it.
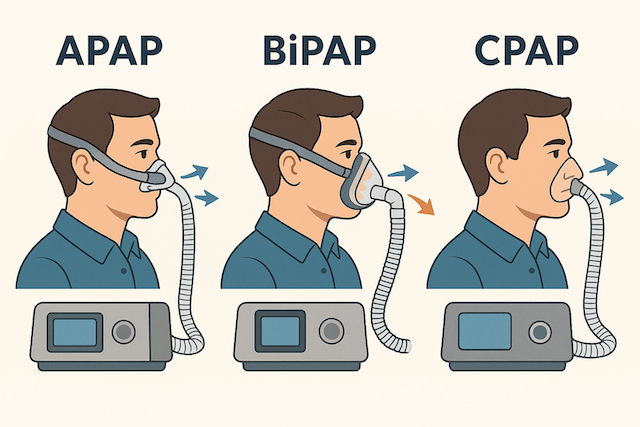
Fixed Pressure vs Auto-Adjusting
The machine I use is an auto-adjusting CPAP, sometimes called APAP. Rather than delivering the same fixed pressure all night, it monitors my breathing continuously and adjusts the pressure up or down in real time based on what my airway needs at any given moment. On nights when I’m congested or sleeping on my back, the pressure might climb to 12. When I’m on my side and breathing smoothly, it settles around 8. The machine makes those adjustments without waking me.
A standard fixed-pressure CPAP does what it says: one prescribed pressure all night. For people with consistent, predictable sleep apnea that doesn’t vary much with position or sleep stage, this works perfectly well and is simpler. I started on a fixed-pressure machine and it was fine. The auto-adjusting version has the advantage of not delivering more pressure than you need at any given moment, which some people find more comfortable, and of adapting to changes like congestion or weight fluctuation without needing a prescription adjustment.
If you need significantly higher exhalation pressure than you can comfortably breathe against, a BiPAP machine, which uses separate settings for inhaling and exhaling, is worth discussing with your sleep specialist. I haven’t needed one, but plenty of people find it much more comfortable than standard CPAP. My CPAP vs BiPAP comparison covers the differences in more detail.
The Features That Actually Matter
After ten years I have clear views on which features make a real difference and which ones you can ignore.
The ramp function is genuinely useful, especially in the early stages of therapy. It lets the machine start at a lower pressure when you first put the mask on and gradually build up to your prescribed level over the following fifteen to thirty minutes while you fall asleep. I use a twenty-minute ramp every single night. Starting at full pressure the moment you put the mask on feels intrusive. The ramp removes that.
EPR, which stands for Expiratory Pressure Relief, reduces the pressure slightly when you breathe out, making exhalation feel more natural. Breathing out against constant pressure takes getting used to, and EPR smooths that out. I have mine set to level 2 on the ResMed, meaning the pressure drops by 2 cmH₂O on each exhale, and I’d feel its absence immediately if I turned it off.
The data tracking has been one of the things I’ve engaged with most deeply. My machine syncs overnight with the ResMed myAir app, which gives me a daily score based on my AHI, hours of use, mask seal, and events. For more detailed analysis I use OSCAR software, which reads the raw data from the SD card and lets me see everything in granular detail. Understanding your data, knowing whether your therapy is actually working on any given night, is one of the things that turns you from a passive patient into someone who actively manages their treatment. The guide to interpreting CPAP data I wrote walks through how to read the numbers without needing a medical background.
The Mask Question
The mask is where most people’s CPAP experience is won or lost. I’ve tried somewhere around fifteen different masks over the years. I use a full face mask now, covering both nose and mouth, because I’m a mouth breather and a nasal mask alone doesn’t work for me. The pressurised air would simply escape through my mouth and the therapy would be ineffective. If you breathe through your nose consistently a nasal mask or nasal pillows will likely be more comfortable, as they’re smaller and less intrusive.
Getting the fit right matters more than almost anything else. A mask that leaks, even slightly, reduces how effective the therapy is and can dry out your eyes if the air is escaping toward your face. I fit my mask while lying down in my actual sleeping position because what seals perfectly sitting upright in front of a mirror can open up completely when you turn on your side. I also use mask liners, which sit between your skin and the cushion and improve both the seal and the skin irritation that some people get from prolonged contact with the silicone.
A CPAP pillow with cutouts for the mask made a noticeable difference to my leak rate when I started side sleeping more. It sounds like a minor thing but it reduced the number of times the mask was being pushed out of position by the pillow through the night.
What It Felt Like to Start
My first night with CPAP I got about three hours of broken sleep. The mask felt strange, the pressure felt intrusive, and I kept waking up aware of the apparatus on my face. By the third or fourth night something started to shift. By the end of the second week I was sleeping through more consistently. Now I can’t sleep comfortably without it.
What sustained me through those early nights was knowing what the morning after a properly treated night would feel like. I’d had my titration night in the sleep lab where they fitted me with a mask during the second half of the night and adjusted the pressure until my apneas stopped. I woke up that morning more alert than I’d felt in years. That single data point, knowing that this was what treated sleep felt like, made the adjustment period feel like a temporary inconvenience rather than a reason to give up.
The Mayo Clinic’s guidance on common CPAP problems is worth reading if you’re in the early stages and hitting difficulties. Most of the common issues, dry mouth, mask leaks, rainout, pressure discomfort, have practical solutions and are not reasons to conclude that CPAP isn’t going to work for you.
What It Does to Your Body Over Time
My AHI on therapy sits under 2. Down from 51 before treatment. My overnight oxygen stays in the healthy range throughout the night rather than dropping into the seventies. My blood pressure normalised within a few months of starting. The migraines that were arriving every single morning stopped the day after my first treated night and haven’t returned.
The Cleveland Clinic describes CPAP as one of the most effective treatments available for obstructive sleep apnea, and the decade I’ve spent using it gives me no reason to disagree. The machine sitting on my nightstand is filtering and pressurising room air, maintaining exactly enough pressure in my airway to keep it from collapsing, and preventing the oxygen deprivation that was doing cumulative damage to my heart and brain for years before I was diagnosed.
That’s what it does. Every night. And that’s why I keep using it.
⚠️ MEDICAL DISCLAIMER This blog provides general information only and is not a substitute for professional medical advice, diagnosis, or treatment. Sleep apnea is a serious condition, and CPAP equipment should be used under proper medical supervision. Always consult your doctor or sleep specialist before starting, stopping, or changing any therapy. I share personal experiences as a CPAP user, not as a medical professional. Individual results vary. For medical guidance, please consult a qualified clinician or the American Academy of Sleep Medicine (aasm.org).