Difference Between APAP, BiPAP, and CPAP: I Break it Down
If you’ve been diagnosed with sleep apnea, you’ve probably heard terms like CPAP, BiPAP, and APAP thrown around by your doctor or sleep specialist.
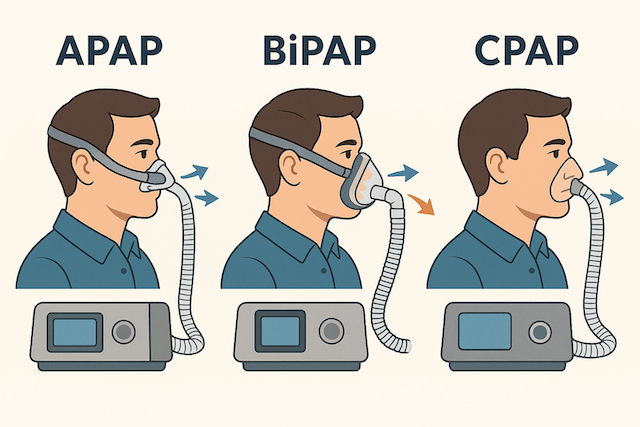
These acronyms can be confusing, and understanding the differences between these therapies is crucial for choosing the right treatment and getting the best results.
In this comprehensive guide, I’ll break down everything you need to know about these three types of positive airway pressure (PAP) therapy, including how they work, when each is used, their advantages and disadvantages, and which might be best for your specific situation.
Medical Disclaimer: The information provided in this article is for educational purposes only and is not intended to replace professional medical advice, diagnosis, or treatment. Always consult with a qualified healthcare provider or sleep specialist to determine the appropriate treatment for your individual needs.
Understanding Positive Airway Pressure (PAP) Therapy
Before diving into the specific differences between APAP, BiPAP, and CPAP, it’s important to understand the fundamental concept behind all these therapies: positive airway pressure.
What Is PAP Therapy?
Positive airway pressure therapy uses a machine to deliver pressurized air through a tube connected to a mask worn over your nose, mouth, or both. According to the Sleep Foundation, this pressurized air works like a pneumatic splint, keeping your upper airway open during sleep and preventing the breathing interruptions that characterize sleep apnea.
PAP therapy is considered the gold standard treatment for obstructive sleep apnea (OSA) and is also used for central sleep apnea (CSA) and complex sleep apnea.
The Basic Components
All PAP devices share similar components:
- Machine: Generates and regulates the pressurized air
- Tubing: Delivers air from the machine to the mask (standard or heated CPAP tubing)
- Mask: Interface that delivers air to your airway (comes in various CPAP mask types)
- Humidifier: Most modern machines include a CPAP humidifier to prevent dryness
- Filter: Ensures clean air delivery
Understanding how a CPAP machine works provides the foundation for understanding the variations between different PAP therapies.
CPAP: Continuous Positive Airway Pressure
What Is CPAP?
CPAP (Continuous Positive Airway Pressure) is the most common and widely studied form of PAP therapy. As the name suggests, CPAP delivers a continuous, steady stream of pressurized air at one fixed pressure level throughout the night.
How CPAP Works
CPAP machines maintain the same pressure whether you’re inhaling or exhaling. The pressure is measured in centimeters of water pressure (cm H2O), and typical CPAP settings range from 4 to 20 cm H2O, with the average prescription falling between 8 to 10 cm H2O.
Here’s what happens when you use CPAP:
- You fall asleep wearing the mask connected to the machine
- The machine generates a constant flow of pressurized air
- The air travels through the tubing into your mask
- The pressure keeps your airway open by preventing the soft tissues in your throat from collapsing
- You breathe normally throughout the night without apnea episodes
The pressure level is determined during a CPAP titration study or CPAP sleep study, where sleep specialists find the optimal pressure needed to eliminate your breathing disruptions.
When Is CPAP Prescribed?
CPAP is typically the first-line treatment for:
- Obstructive sleep apnea: When your airway becomes physically blocked during sleep
- Mild to severe OSA: Regardless of severity, CPAP is usually tried first
- Patients without complicating factors: Those without significant lung disease or heart failure
Sleep apnea diagnosis usually leads to CPAP therapy as the initial recommendation because it’s the most researched, cost-effective, and successful treatment for the majority of patients.
Advantages of CPAP
1. Proven Effectiveness: Decades of research confirm CPAP’s effectiveness in treating sleep apnea
2. Cost-Effective: Generally less expensive than BiPAP or APAP machines
3. Widely Available: Most insurance companies cover CPAP therapy, and there are many CPAP machine types available
4. Simpler Technology: Fewer moving parts and settings mean less can go wrong
5. Extensive Product Options: From best CPAP machines to specialized equipment like travel CPAP machines
6. Insurance Coverage: Most insurance plans readily cover CPAP as a first-line treatment
7. Long-Term Data: Extensive studies on CPAP therapy’s long-term benefits
Disadvantages of CPAP
1. Single Pressure Level: Some people find it difficult to exhale against the constant incoming pressure
2. Discomfort: The continuous pressure can feel unnatural, especially for new users
3. Common Side Effects:
4. Adaptation Period: Many users struggle during their first night with CPAP and need time to adjust
5. Compliance Challenges: Maintaining CPAP compliance can be difficult
Modern CPAP Features
Today’s CPAP machines often include comfort features:
- Ramp Function: Starts at a lower pressure and gradually increases
- EPR (Expiratory Pressure Relief): Slightly reduces pressure during exhalation
- Integrated Humidification: Prevents dryness
- Data Tracking: Monitors usage and effectiveness (can be analyzed with OSCAR CPAP software)
- Quiet Operation: Modern machines are nearly silent
Popular CPAP Models
Check out reviews of specific machines:

- ResMed AirSense 11 AutoSet (show above)
- ResMed AirSense 10 AutoSet
APAP: Auto-Adjusting Positive Airway Pressure
What Is APAP?
APAP (Auto-Adjusting Positive Airway Pressure), also called Auto-CPAP or Auto-PAP, represents a significant technological advancement over traditional CPAP. Instead of delivering a single fixed pressure, APAP machines continuously monitor your breathing and automatically adjust the pressure throughout the night.
How APAP Works
According to research published in Sleep and Breathing, APAP devices use sophisticated algorithms to detect breathing patterns and adjust pressure in real-time. Here’s the process:
- Continuous Monitoring: The machine monitors your breathing through sensors that detect:
- Airflow patterns
- Snoring
- Apnea events
- Hypopnea (shallow breathing)
- Airway resistance
- Automatic Adjustments: When the algorithm detects breathing problems, it increases pressure to prevent apnea episodes
- Pressure Reduction: When breathing normalizes, the machine decreases pressure to the minimum needed
- Pressure Range: Your doctor sets a minimum and maximum pressure range (typically 4-20 cm H2O), and the machine operates within these limits
The key advantage? According to SleepApnea.org, APAP provides higher pressure when you need it (such as during REM sleep or when sleeping on your back) and lower, more comfortable pressure when you don’t.
Understanding How Auto-CPAP Works
The sophisticated algorithms in APAP machines respond to:
- Sleep Position: You may need more pressure on your back than on your side
- Sleep Stages: REM sleep often requires higher pressure than other sleep stages
- Nasal Congestion: Temporary congestion may require pressure adjustments
- Weight Changes: Pressure needs may vary with weight fluctuations
- Alcohol Consumption: Affects muscle tone and pressure requirements
Research from the Journal of Clinical Sleep Medicine indicates that APAP effectively determines the optimal pressure for 90-95% of total sleep time.
When Is APAP Prescribed?
APAP may be recommended for:
- Variable Pressure Needs: Patients whose pressure requirements change throughout the night
- Positional Sleep Apnea: Those whose apnea severity depends on sleep position
- REM-Related Sleep Apnea: Patients who primarily have apneas during REM sleep
- Weight Fluctuations: People experiencing ongoing weight changes
- CPAP Intolerance: Those who find fixed CPAP pressure uncomfortable
- Uncertain Pressure Needs: When optimal pressure hasn’t been determined through a sleep study
- Nasal Congestion Issues: Patients with allergies or variable nasal resistance
Advantages of APAP
1. Comfort: Lower average pressure throughout the night compared to CPAP
2. Flexibility: Adapts to changing needs without requiring adjustment or re-titration
3. Effective Pressure Delivery: Provides exactly what you need, when you need it
4. Potentially Better Compliance: Some studies suggest improved adherence due to comfort
5. No Titration Study Needed: Can be prescribed after a home sleep apnea test without in-lab titration
6. Can Function as CPAP: Most APAP machines can be set to deliver fixed pressure if needed
7. Better for Variable Conditions: Adapts to changes in sleep position, congestion, or other factors
Disadvantages of APAP
1. Cost: Generally more expensive than standard CPAP machines
2. Algorithm Variability: Different manufacturers use different algorithms with varying effectiveness
3. Potential for Pressure Fluctuations: Constant adjustments may disrupt some people’s sleep
4. Complexity: More sophisticated technology means more potential points of failure
5. Not Suitable for Everyone: According to PMC research, APAP is recommended only for otherwise healthy OSA patients
6. Insurance Coverage: Some insurance companies may not cover APAP as readily as CPAP
7. Learning Curve: Requires understanding of pressure settings and data interpretation
APAP vs CPAP: What the Research Shows
According to a meta-analysis published in PMC, APAP and CPAP show:
- Equivalent effectiveness in reducing apnea-hypopnea index (AHI)
- Similar adherence rates in most studies
- Lower mean pressure with APAP (potentially more comfortable)
- No clinically significant difference in improvement of sleepiness or quality of life
However, research also suggests that some patients may experience better outcomes with one versus the other, particularly those with lighter sleep who may be more sensitive to pressure fluctuations.
BiPAP: Bilevel Positive Airway Pressure
What Is BiPAP?
BiPAP (Bilevel Positive Airway Pressure), also called BPAP or bilevel PAP, delivers two different pressure levels: one when you inhale and a lower pressure when you exhale.
Note: BiPAP is technically a brand name from Respironics (similar to how Kleenex is a brand of tissue), but it has become the commonly used term for all bilevel PAP devices.
How BiPAP Works
SleepApnea.org explains that BiPAP provides:
IPAP (Inspiratory Positive Airway Pressure): Higher pressure delivered when you breathe in EPAP (Expiratory Positive Airway Pressure): Lower pressure delivered when you breathe out
For example, a BiPAP setting might be:
- IPAP: 14 cm H2O (inhalation)
- EPAP: 10 cm H2O (exhalation)
This difference in pressure makes it easier to exhale while still maintaining enough pressure to keep your airway open.
According to Apria Healthcare, BiPAP machines have a typical pressure range of 4 to 30 cm H2O—a wider range than standard CPAP.
Types of BiPAP Modes
BiPAP machines can operate in different modes:
1. Spontaneous (S) Mode: Detects when you breathe and switches between IPAP and EPAP automatically
2. Timed (T) Mode: Delivers a set number of breaths per minute regardless of your breathing
3. Spontaneous/Timed (S/T) Mode: Allows you to breathe on your own but delivers backup breaths if needed
4. Auto BiPAP: Automatically adjusts both IPAP and EPAP based on your breathing patterns
Learn more about what a BiPAP machine is and explore the best BiPAP machines available.
When Is BiPAP Prescribed?
BiPAP is typically recommended for:
1. CPAP Intolerance: Patients who cannot tolerate exhaling against constant CPAP pressure
2. High-Pressure Requirements: Those needing pressure settings above 15-20 cm H2O
3. Central Sleep Apnea: Patients with central sleep apnea may benefit from BiPAP’s breathing support
4. Complex Sleep Apnea: Those with complex or mixed sleep apnea that combines obstructive and central elements
5. Cheyne-Stokes Respiration: A specific breathing pattern often seen with heart failure
6. Obesity Hypoventilation Syndrome: Also called Pickwickian Syndrome, where breathing becomes too shallow
7. Chronic Lung Disease: Patients with COPD or other restrictive lung diseases who need help moving air in and out
8. Neuromuscular Disorders: Conditions affecting breathing muscles
9. Heart Failure: Patients with heart conditions who need respiratory support
10. Low Oxygen Levels: Those who experience significant oxygen desaturation during sleep
Advantages of BiPAP
1. Easier Exhalation: Lower pressure on exhale makes breathing feel more natural
2. Better for High Pressures: More comfortable when high pressures are needed
3. Ventilatory Support: Helps move air in and out of lungs, not just keeping airway open
4. Versatility: Can treat more complex breathing problems beyond simple OSA
5. Multiple Modes: Different settings for various medical conditions
6. Higher Pressure Range: Can deliver pressures up to 30 cm H2O
7. Backup Breathing: Some modes provide breaths if you stop breathing
Disadvantages of BiPAP
1. Cost: Significantly more expensive than CPAP machines
2. Complexity: More settings to adjust and manage
3. Insurance Coverage: May require medical justification and prior authorization
4. Not First-Line Treatment: Usually only prescribed after CPAP has been tried and failed
5. Similar Side Effects: Can still cause dry mouth, mask leaks, and other common PAP issues
6. Overkill for Simple OSA: Most people with uncomplicated OSA don’t need BiPAP’s advanced features
7. Learning Curve: Takes more time to adjust to than CPAP
Popular BiPAP Models
Check out reviews of specific machines:

- Luna G3 BiPAP 25A Review (shown above)
APAP vs BiPAP vs CPAP: Direct Comparison
Comparison Chart
| Feature | CPAP | APAP | BiPAP |
|---|---|---|---|
| Pressure Delivery | Single fixed pressure | Variable pressure within a range | Two pressure levels (in/out) |
| Typical Range | 4-20 cm H2O | 4-20 cm H2O | 4-30 cm H2O |
| Cost | $ | $$ | $$$ |
| Complexity | Simple | Moderate | Complex |
| Best For | Most OSA patients | Variable pressure needs | High pressures, CSA, complex cases |
| Insurance Coverage | Excellent | Good | May require justification |
| Comfort | Adequate | Better (variable pressure) | Best (easier exhalation) |
| Technology | Basic | Advanced algorithms | Most sophisticated |
| Common Uses | First-line OSA treatment | OSA with variable needs | CSA, high pressure needs, COPD |
Which Therapy Is Right for You?
The answer depends on multiple factors:
Choose CPAP if you:
- Have straightforward obstructive sleep apnea
- Tolerate the single pressure level
- Want the most cost-effective option
- Prefer simplicity
- Need maximum insurance coverage likelihood
Choose APAP if you:
- Have variable pressure needs throughout the night
- Experience positional sleep apnea
- Want optimal comfort
- Have REM-related sleep apnea
- Need flexibility for changing conditions
- Couldn’t tolerate CPAP due to pressure discomfort
Choose BiPAP if you:
- Cannot tolerate CPAP or APAP
- Require high-pressure settings (>15 cm H2O)
- Have central or complex sleep apnea
- Have coexisting lung disease
- Need ventilatory support
- Experience significant difficulty exhaling against pressure
Understanding ASV vs BiPAP vs CPAP
For completeness, it’s worth mentioning ASV (Adaptive Servo-Ventilation), an even more advanced therapy:
What Is ASV?
ASV (Adaptive Servo-Ventilation) is the most sophisticated form of PAP therapy. It’s specifically designed for:
- Complex sleep apnea
- Central sleep apnea
- Cheyne-Stokes respiration with heart failure
ASV machines continuously analyze your breathing patterns and provide customized pressure support on a breath-by-breath basis. Unlike BiPAP, which delivers predetermined pressure levels, ASV adapts in real-time to maintain stable breathing patterns.
Popular ASV Machines
Check out reviews of specific machines:

- ResMed AirCurve 11 ASV Review (shown above)
- ResMed AirCurve 10 ASV Review
Learn more about how ASV works and the potential ASV therapy for other health conditions.
Making the Transition: Switching Between Devices
From CPAP to APAP
Many sleep specialists now start patients directly on APAP, as research shows comparable outcomes with potentially better comfort. If you’re switching from CPAP to APAP:
- Your pressure settings will be converted to a range
- The machine will likely determine an average pressure similar to your fixed CPAP setting
- You may notice the pressure feels more variable
From CPAP/APAP to BiPAP
This switch typically happens when:
- You cannot tolerate CPAP/APAP despite adjustments
- Your pressure needs have increased significantly
- You’ve developed central sleep apnea events (treatment-emergent central sleep apnea)
- You have coexisting medical conditions requiring BiPAP
Understanding the difference between APAP, BiPAP, and CPAP helps prepare you for transitions.
Getting Started with PAP Therapy
Initial Setup and Titration
Regardless of which PAP device you use, proper setup is crucial:
1. Sleep Study: Most patients undergo a diagnostic sleep study to confirm sleep apnea
2. Pressure Determination: Through CPAP titration or using APAP for automatic titration
3. Mask Fitting: Critical for success – choosing the right CPAP mask prevents leaks and discomfort
4. Education: Learning how to use a CPAP machine properly
5. Follow-Up: Regular monitoring to ensure effectiveness and CPAP compliance
Mask Options for All PAP Devices
All PAP therapies use similar mask interfaces:
- Nasal Masks: Cover only the nose (best CPAP nasal masks)
- Nasal Pillow Masks: Seal at nostrils (difference between nasal pillow and nasal mask)
- Full Face Masks: Cover both nose and mouth (best full face CPAP masks)
- Specialized Masks: For side sleepers (best mask for side sleepers), stomach sleepers (best mask for stomach sleepers), beards (best mask for beards), and more
Overcoming Common Challenges
Starting PAP therapy can be challenging. Here’s how to address common issues:
Difficulty Adapting:
- Read how to get used to CPAP therapy
- Start with short wearing sessions while awake
- Use the ramp feature
- Consider overcoming CPAP anxiety
Dry Mouth or Nose:
- Use heated humidification
- Ensure proper mask fit
- Try chin straps for mouth breathers
- Consider masks for mouth breathers (best masks for mouth breathers)
Mask Issues:
- Experiment with different mask styles
- Use mask liners to prevent irritation
- Try strap covers for comfort
- Learn to prevent mask lines
Air Leaks:
- Ensure proper mask fit
- Check for worn components
- Adjust straps (not too tight!)
Claustrophobia:
- Try different mask styles (nasal pillows may feel less restrictive)
- Practice wearing mask while awake
- Use desensitization techniques
For more strategies, see how to sleep better with sleep apnea.
Maintenance and Care
All PAP devices require regular maintenance:
Daily Tasks:
- Empty and rinse the water chamber
- Wipe the mask and cushion
- Hang the tubing to air dry
Weekly Tasks:
- Wash mask, headgear, and tubing with mild soap
- Clean the water chamber thoroughly
- Check for wear and damage
Monthly Tasks:
- Replace disposable filters
- Inspect all components for wear
Replacement Schedule:
Follow the CPAP replacement schedule:
- Mask cushions: Every 2-4 weeks
- Mask: Every 3-6 months
- Tubing: Every 3 months
- Filters: Monthly (disposable) or as needed (reusable)
- Water chamber: Every 6 months
Learn about CPAP cleaning supplies and how to clean a CPAP machine.
Cost Considerations
Price Ranges (Without Insurance)
CPAP Machines: $500-$1,000
- Most affordable option
- Widely available
- Proven technology
APAP Machines: $700-$1,200
- Mid-range pricing
- Advanced features
- Auto-adjusting capability
BiPAP Machines: $1,500-$3,000+
- Most expensive
- Sophisticated technology
- Medical-grade ventilation
Insurance Coverage
Most health insurance plans, including Medicare and Medicaid, cover PAP therapy for diagnosed sleep apnea. However:
CPAP: Usually covered with minimal documentation
APAP: Generally covered, may require justification
BiPAP: Often requires:
- Documentation of CPAP failure
- Medical necessity from a physician
- Prior authorization
- Proof of specific medical conditions
Understanding CPAP insurance compliance helps maintain coverage.
Monitoring Your Therapy
Tracking Your Progress
Modern PAP machines collect detailed data:
- Hours of use: Tracking CPAP compliance
- AHI (Apnea-Hypopnea Index): Number of events per hour
- Mask leak: Amount and duration of leaks
- Pressure levels: Average and maximum pressures used
Learning to interpret CPAP data helps you understand your treatment effectiveness.
Signs Your Therapy Is Working
You should notice:
- Decreased daytime sleepiness (check Epworth Sleepiness Scale)
- More energy during the day
- Better concentration and memory
- Improved mood
- Reduced morning headaches
- Better cardiovascular health
- Potential improvements in sleep apnea and mental health
When to Contact Your Doctor
Reach out to your sleep specialist if you experience:
- Persistent daytime sleepiness despite therapy
- High AHI or leak rates
- Continued snoring
- Difficulty tolerating the device
- New or worsening symptoms
- Equipment malfunctions
Troubleshooting CPAP problems can help resolve many issues independently.
Special Considerations
Traveling with PAP Devices
All PAP types can be used while traveling:
- Standard machines may require a travel CPAP bag
- Mini travel CPAP machines available (my mini CPAP travel machine)
- Learn the best ways to travel with CPAP
- Consider CPAP batteries for camping or areas without electricity
Using PAP with Other Conditions
When Sick: Guidelines for using CPAP when sick
Without Water: Information on using CPAP without water
Deviated Septum: Special considerations for those with deviated septums
Mouth Breathing: Solutions for preventing mouth breathing with CPAP
Gender-Specific Considerations
For Women:
- Sleep apnea in women presents differently
- CPAP machines for women may offer smaller masks
- Best CPAP masks for women
For Children:
- Sleep apnea in children requires different approaches
- Best CPAP masks for children
- Does my child have sleep apnea?
Alternative and Complementary Treatments
While PAP therapy is the gold standard, other options exist:
Alternative Treatments
Learn about alternative treatments for sleep apnea:
- Oral Appliances: Sleep apnea mouth guards
- Positional Therapy: Positional therapy for sleep apnea
- Surgery: Various sleep apnea surgery options
- Hypoglossal Nerve Stimulation: Inspire treatment
- EPAP Therapy: EPAP devices as alternatives
Lifestyle Modifications
Important complementary approaches:
- Weight Loss: Reversing sleep apnea naturally
- Exercise: Regular physical activity
- Sleep Position: Best sleeping positions
- Avoiding Alcohol: Especially before bed
- Nasal Health: Addressing congestion
When PAP Therapy Isn’t Enough
Some patients may need additional interventions beyond PAP therapy, especially those with:
- Complex medical conditions: Multiple comorbidities
- Treatment-resistant sleep apnea: Despite optimal PAP therapy
- Overlap Syndrome, which is a combination of COPD and OSA
Long-Term Outlook and Benefits
Health Benefits of Successful PAP Therapy
Proper treatment provides numerous benefits:
Cardiovascular:
- Reduced stroke risk
- Lower blood pressure
- Decreased risk of heart attack
- Improved cardiovascular health
Metabolic:
- Better blood sugar control
- Improved insulin sensitivity
- Support for weight loss efforts
Cognitive:
- Reduced brain fog
- Better memory and concentration
- Lower risk of brain damage from untreated sleep apnea
Quality of Life:
- Increased energy
- Better mood
- Improved sexual health
- Reduced nighttime urination
- Enhanced overall living with sleep apnea
Maintaining Long-Term Success
Keys to staying consistent with CPAP therapy:
- Make it part of your routine
- Address problems promptly
- Keep equipment clean and maintained
- Stay connected with your healthcare team
- Track your progress
- Celebrate improvements
Emerging Technologies and Future Developments
The field of sleep medicine continues to evolve:
Innovations on the Horizon
- Improved Algorithms: More responsive and personalized pressure delivery
- Smaller Devices: Continued miniaturization of PAP machines
- Better Data Analysis: AI-powered insights from therapy data
- Pharmacological Options: Sleep apnea pills in development
- Enhanced Comfort Features: New mask designs and humidification systems
- Future of ASV Technology: More sophisticated adaptive ventilation
Current Alternatives Being Researched
- Weight loss medications like Zepbound for sleep apnea
- Advanced surgical techniques
- Combination therapies
- Personalized medicine approaches
Frequently Asked Questions
Can I switch between CPAP, APAP, and BiPAP?
Yes, but only with your doctor’s approval. Many patients try CPAP first, then switch to APAP or BiPAP if needed. Some people also switch back from APAP to CPAP if they prefer fixed pressure.
Which is more effective: CPAP or APAP?
Research shows they’re equally effective at reducing sleep apnea events. APAP may be more comfortable for some people, but this varies by individual.
Why would someone need BiPAP instead of CPAP?
BiPAP is typically prescribed when someone cannot tolerate CPAP, needs very high pressures, has central sleep apnea, or has coexisting lung disease requiring ventilatory support.
Are the masks different for CPAP, APAP, and BiPAP?
No, all three types use the same mask styles and interfaces. The difference is in how the machine delivers pressure, not in the mask design.
How long does a PAP machine last?
With proper care, CPAP machines typically last 3-5 years. Insurance often covers replacement every 5 years.
Can I adjust my own pressure settings?
You should never adjust pressure settings without consulting your doctor. Incorrect pressure can be ineffective or potentially dangerous.
Do I need a prescription for APAP, BiPAP, or CPAP?
Yes, all PAP devices require a prescription from a licensed healthcare provider. This ensures proper diagnosis and appropriate treatment.
What if I can’t tolerate any PAP therapy?
Discuss alternatives with your doctor, including oral appliances, positional therapy, surgery, or hypoglossal nerve stimulation. Alternative treatments are available.
Conclusion
Understanding the differences between APAP, BiPAP, and CPAP is essential for making informed decisions about your sleep apnea treatment. While the acronyms can be confusing, the basic concepts are straightforward:
CPAP delivers one continuous pressure—simple, effective, and affordable for most people with obstructive sleep apnea.
APAP automatically adjusts pressure throughout the night—offering flexibility and potentially better comfort for those with variable needs.
BiPAP provides two pressure levels for inhalation and exhalation—ideal for those who need high pressures or have complex breathing problems.
The “best” choice depends entirely on your individual needs, medical conditions, tolerance, and preferences. Most patients start with CPAP or APAP, and only move to BiPAP if medically necessary.
Remember:
- Work closely with your sleep specialist to find the right therapy
- Give yourself time to adapt—it often takes weeks to adjust
- Address problems early rather than suffering in silence
- Maintain your equipment properly
- Track your progress and celebrate improvements
With the right device and proper support, PAP therapy can dramatically improve your sleep quality, health, and overall quality of life. The journey may have challenges, but the destination—restorative, healthy sleep—is well worth it.
If you’re struggling with your current PAP therapy or wondering if a different device might work better, don’t hesitate to talk to your healthcare provider. Treatment should be tailored to you, and options exist to make therapy comfortable and effective.
About This Article: This comprehensive guide comparing APAP, BiPAP, and CPAP was researched using information from peer-reviewed medical journals, leading health organizations, and sleep medicine experts. For personalized advice about your sleep apnea treatment, always consult with a qualified healthcare provider or board-certified sleep specialist.
Related Reading:
- What Is Sleep Apnea?
- Sleep Apnea Treatment Options
- CPAP vs BiPAP: Detailed Comparison
- Obstructive Sleep Apnea
- Central Sleep Apnea
- How to Choose a CPAP Mask
References and Medical Sources
- Sleep Foundation – “BiPAP vs. CPAP Machines: Breaking Down the Differences” – https://www.sleepfoundation.org/cpap/cpap-vs-bipap
- Healthline – “APAP vs. CPAP vs. BiPAP: How Sleep Apnea Therapies Differ” – https://www.healthline.com/health/apap-vs-cpap
- SleepApnea.org – “APAP vs. CPAP: Which Is Better for Sleep Apnea?” – https://www.sleepapnea.org/cpap/apap-vs-cpap/
- SleepApnea.org – “BiPAP vs. CPAP: Differences in Positive Airway Pressure Therapy” – https://www.sleepapnea.org/cpap/cpap-vs-bipap/
- Apria Healthcare – “CPAP vs BiPAP: What’s the Difference?” – https://www.apria.com/home-healthcare-insights/cpap-and-bipap
- Sleep and Breathing (Springer) – “Auto-adjusting positive airway pressure: the fine line between engineering and medicine” – https://link.springer.com/article/10.1007/s11325-025-03409-w
- Journal of Clinical Sleep Medicine – “Auto-adjusting Positive Airway Pressure Treatment for Sleep Apnea Diagnosed by Home Sleep Testing” – https://jcsm.aasm.org/doi/10.5664/jcsm.4272
- PMC/National Library of Medicine – “Less may be more: CPAP vs. APAP in the treatment of obstructive sleep apnea” – https://pmc.ncbi.nlm.nih.gov/articles/PMC8836615/
- PMC/National Library of Medicine – “Auto-adjusting positive airway pressure: the fine line between engineering and medicine” – https://pmc.ncbi.nlm.nih.gov/articles/PMC12304072/
- PMC/National Library of Medicine – “Comparative assessment of several automatic CPAP devices’ responses: a bench test study” – https://pmc.ncbi.nlm.nih.gov/articles/PMC5005142/
- American Journal of Respiratory and Critical Care Medicine – “Comparison between Automatic and Fixed Positive Airway Pressure Therapy in the Home” – https://www.atsjournals.org/doi/10.1164/rccm.200201-022OC
- Houston ENT Doctor – “CPAP vs. BiPAP vs. APAP: Which Is Best?” – https://breathefreely.com/cpap-vs-bipap-vs-apap-which-is-best/
- SleepQuest – “CPAP vs BiPAP vs APAP: Choosing the Right Sleep Therapy Device” – https://shop.sleepquest.com/blog/cpap-vs-bipap-vs-apap-choosing-the-right-sleep-therapy-device/
- CPAP.com – “BiPAP Machine vs APAP Machine: Differences and Uses of Both” – https://www.cpap.com/blogs/cpap-therapy/bipap-machine-apap-machine-differences-both
- PubMed/NCBI – “Comparison of three auto-adjusting positive pressure devices in patients with sleep apnoea” – https://pubmed.ncbi.nlm.nih.gov/16571610/
Medical Review Note: Information in this article is sourced from peer-reviewed medical literature, academic medical centers, and reputable health organizations. Last reviewed: November 2025.
⚠️ MEDICAL DISCLAIMER This blog provides general information only and is not a substitute for professional medical advice, diagnosis, or treatment. Sleep apnea is a serious condition, and CPAP equipment should be used under proper medical supervision. Always consult your doctor or sleep specialist before starting, stopping, or changing any therapy. I share personal experiences as a CPAP user, not as a medical professional. Individual results vary. For medical guidance, please consult a qualified clinician or the American Academy of Sleep Medicine (aasm.org).




