Best CPAP Masks for Mouth Breathers
“This post contains affiliate links. I may earn a commission if you buy through these links, at no extra cost to you. Read my Disclaimer for more details.”
When I sleep, I’m a mouth breather. I was diagnosed with severe sleep apnea over 10 years ago.

My sleep specialist started me on the ResMed AirFit F20 full-face mask straight away because I’m usually congested, so I tend to breathe through my mouth. Smart move on her part.
The F20 worked from night one. I could breathe naturally with my mouth open, the seal held perfectly, and my AHI dropped to under 4. I’ve used the same mask design for over 10 years now because it just works. When something solves your sleep apnea this effectively, you don’t mess with it.
If you’re a mouth breather, whether from nasal congestion, a deviated septum, or just how you naturally breathe, choosing the right mask type from the start makes all the difference.
If you’re wondering. No, I haven’t had the same mask for 10+ years. I get a replacement about every 3 months.
Why Mouth Breathers Need Different CPAP Masks
Here’s what nobody tells you upfront: most CPAP masks are designed for people who breathe through their nose. If you’re a mouth breather using a nasal mask, you’re essentially trying to fill a bucket with a hole in the bottom.
When you breathe in through your nose, but your mouth drops open during sleep, all that therapeutic pressure escapes. Your CPAP machine cranks up the pressure trying to compensate, creating even more air leaks. You wake up with dry mouth, sore throat, high AHI readings, and zero improvement in your sleep quality.
Research shows that mouth breathing during CPAP therapy can reduce treatment efficacy by up to 60% and is one of the leading causes of CPAP compliance failure. The American Academy of Sleep Medicine specifically recommends full-face or hybrid masks for patients who primarily breathe through their mouths.
Common Signs You’re a Mouth Breather
You might be a mouth breather if you:
- Wake up with a dry mouth, cracked lips, or a sore throat every morning
- Have chronic nasal congestion or allergies
- Were diagnosed with a deviated septum or enlarged tonsils
- Snore loudly even with your CPAP (indicating mouth leaks)
- Experience high leak rates on your CPAP data
- Find chin straps uncomfortable or ineffective
- Have consistently high AHI despite using CPAP correctly
Research indicates that 40-60% of sleep apnea patients experience some degree of mouth breathing during sleep, particularly those with nasal obstruction. The good news? The right mask completely changes the game.
Best CPAP Masks for Mouth Breathers: My Top Picks
I’m going to be completely honest with you; As I said, I’ve used the ResMed AirFit F20 for over 10 years, and I’ve never needed to change. It worked so well from day one that I had no reason to try anything else. But I’ve done extensive research on other options for people whose needs differ from mine, and I’ll share what I’ve learned from specs, clinical data, and user feedback.
Top CPAP Masks for Mouth Breathers
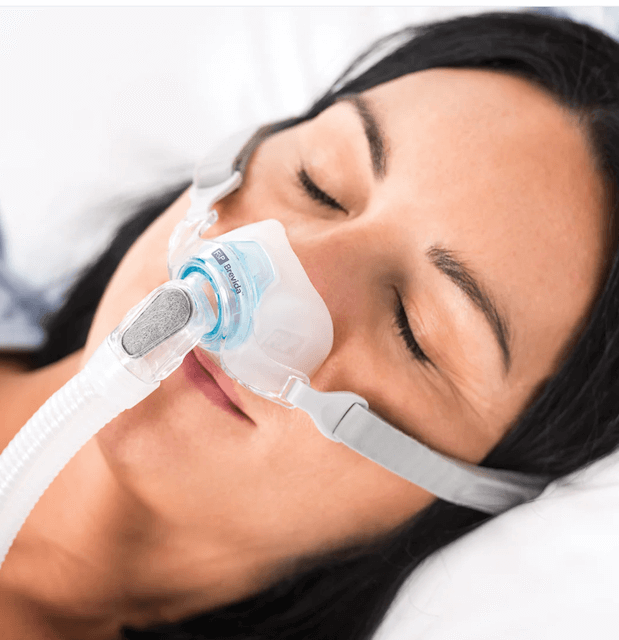
🥇 ResMed AirFit F20 – Best Overall for Mouth Breathers

Yes, this is yours truly modelling the ResMed F20 Full Face Mask!
My Personal Experience: This is the only mask I’ve ever used, and I got lucky that my sleep clinic started me on the right one. They prescribed the F20 from day one since I’m a mouth breather. First night, my AHI dropped to under 4. I’ve used it for 10+ years now and never looked back. The InfinitySeal cushion adapts to my face shape and maintains a seal even when my jaw drops open during REM sleep.
Key Features:
- Full-face design covers both nose and mouth completely
- InfinitySeal cushion technology adapts to facial contours
- Magnetic headgear clips for easy on/off
- No forehead strap reduces the claustrophobic feeling
- Effective at pressure settings from 4-20 cm H2O
- Available in small, medium, and large cushion sizes
Best For: People who need high-pressure settings, move around during sleep, or have prominent facial features.
Limitations: Can feel bulky initially; magnetic clips require distance from pacemakers or metallic implants.
My Verdict: If you’re serious about fixing your mouth breathing issue and actually want CPAP therapy to work, start here. The F20 sealed the deal for me—literally. After 10 years, I’ve never looked back.
You can also read my full AirFit F20 review here
🥈 ResMed AirFit F30 – Best for Claustrophobic Users
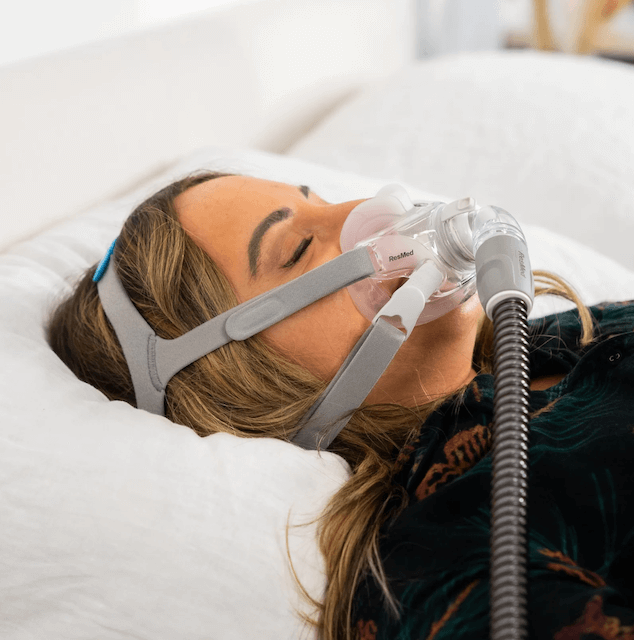
What I’ve Researched: While I haven’t personally used this (the F20 works too well for me to switch), the F30 is essentially a less intimidating version of the F20. It sits under your nose rather than covering the bridge, giving you more field of vision for reading in bed. Based on user reviews and clinical data, this is the “gateway” full-face mask for people transitioning from nasal masks.
Key Features:
- Under-the-nose cushion minimizes facial contact
- Covers the mouth while leaving the bridge of the nose free
- QuietAir vent technology reduces noise to 21 decibels
- Excellent for glasses wearers
- Front-facing connection works for side and back sleepers
Best For: People who feel claustrophobic in traditional full-face masks, wear glasses before bed, or have sensitive skin on the bridge of their nose.
Limitations: Some users report red marks around the mouth seal; limited size options may not fit very large or very small faces.
My Verdict: This is the “gateway” full-face mask for people transitioning from nasal masks. Less intimidating than the F20 but still seals properly for mouth breathers.
🥉 Philips Respironics DreamWear Full Face – Best for Active Sleeper

Great for people who toss and turn. It’s more breathable and doesn’t feel heavy on the face.
What I’ve Researched: The top-of-head tube connection solves a real problem for restless sleepers. Based on user reviews and the design specifications, if you’re someone who frequently moves around or gets tangled in your hose, this innovative placement makes sense.
Key Features:
- Top-of-head tubing eliminates front-of-face hose
- Under-the-nose cushion with full mouth coverage
- 360-degree swivel connection follows movement
- Minimal contact design reduces pressure points
- Available in multiple cushion sizes with a fit-pack option
Best For: Side sleepers, stomach sleepers, people who move frequently during sleep, or anyone who finds traditional hose placement restrictive.
Limitations: Some users find the headgear tighter than other models; the overhead tube design isn’t ideal if you wear a sleep cap or bonnet.
My Verdict: If you’re sick of waking up tangled in your CPAP hose or having it pull your mask off your face, the DreamWear solves that problem instantly.
🏅Fisher & Paykel Vitera – Best for Humidification and Comfort

If you use a heated humidifier, this mask prevents moisture buildup while maintaining comfort.
What I’ve Researched: The RollFit cushion technology on this mask is designed to handle moisture better than standard silicone, which is important if you use high humidification settings. User reviews consistently mention it works well in humid environments or with heated humidifiers.
Key Features:
- RollFit cushion adapts to face shape and movement
- VisiBlue color tint aids proper positioning
- Stability wings prevent sliding during sleep
- Excellent seal retention with heated humidification
- Four-point headgear reduces pressure concentration
Best for: Individuals who use heated humidification, reside in humid climates, or experience CPAP rainout.
Limitations: Larger profile than ResMed F30 or DreamWear; the VisiBlue cushion color is visible in dim light.
My Verdict: Often overlooked but extremely reliable, especially if you crank your humidifier settings. The cushion technology actually improves with humidity rather than degrading.
Understanding CPAP Mask Types: Full-Face vs. Hybrid vs. Nasal
Not all “mouth breather” masks are created equal. Here’s what you actually need to know about different mask categories.
Full-Face Masks: The Traditional Standard
Full-face masks seal from the bridge of your nose down to below your mouth, creating a complete enclosure for both nasal and oral breathing.
Advantages:
- Complete seal regardless of breathing pattern
- Effective for chronic mouth breathers
- Works with high CPAP pressure (15+ cm H2O)
- Solves nasal congestion issues permanently
- No need for chin straps or mouth tape
Disadvantages:
- Can feel claustrophobic initially
- A larger profile interferes with some sleeping positions
- May leave pressure marks if overtightened
- More difficult to sleep on your stomach
Clinical studies show full-face masks reduce mouth leak rates by 85-92% compared to nasal masks in mouth breathers.
Hybrid Masks: Modern Innovation
Hybrid masks combine elements of full-face coverage with the minimalism of nasal cushions. They typically use nasal pillows or under-nose cushions while still covering the mouth.
Advantages:
- Less facial coverage than traditional full-face
- Better field of vision for reading/TV
- Can wear glasses more easily
- Reduced claustrophobic sensation
- Often lighter and more comfortable
Disadvantages:
- May not seal as consistently as a full-face
- Fewer size options available
- It can be more expensive
- Not always compatible with high pressures
Research indicates hybrid masks have similar efficacy to full-face masks for mild-to-moderate mouth breathers but may be less effective in severe cases.
Nasal Masks + Accessories: The Workaround
Some mouth breathers successfully use nasal masks combined with chin straps or mouth tape, though this approach has limitations.
When This Works:
- Mild occasional mouth breathing
- Primary nasal breathing with occasional jaw drop
- Lower pressure requirements (<12 cm H2O)
- Willingness to use additional accessories consistently
When This Fails:
- Chronic mouth breathing
- Significant nasal obstruction
- High-pressure requirements
- Discomfort with chin straps or mouth tape
Many chronic mouth breathers report that chin straps cause jaw pain or discomfort, and mouth tape can feel claustrophobic, especially if nasal congestion develops during sleep. Most severe mouth breathers eventually need a proper full-face solution.
Read more about preventing mouth breathing on CPAP
How to Choose the Right CPAP Mask for Your Mouth Breathing
Beyond just “get a full-face mask,” here are the specific factors that determine which mask will actually work for you long-term.
1. Sleeping Position Matters More Than You Think
Your primary sleeping position dramatically affects which masks will work:
Side Sleepers: Look for low-profile designs like the F30 or DreamWear that don’t have rigid frames extending far from your face. A good CPAP pillow designed with mask cutouts is essential.
Back Sleepers: You have the most flexibility. Any full-face mask will work, though back sleeping can worsen sleep apnea in some patients.
Stomach Sleepers: This is the hardest position for full-face masks. The DreamWear with top-of-head tubing is your best bet. Consider whether adjusting your sleep position might be easier than finding the perfect mask.
Combination Sleepers: Choose masks with 360-degree swivel connections and flexible frames that adapt to position changes. The DreamWear and Vitera handle this well.
2. Pressure Requirements
Your prescribed CPAP pressure affects mask selection:
Low Pressure (4-10 cm H2O): Almost any full-face mask works. Focus on comfort and ease of use.
Medium Pressure (10-15 cm H2O): Most quality full-face masks handle this range. Ensure a good seal with InfinitySeal or RollFit cushion technology.
High Pressure (15-20+ cm H2O): Stick with proven designs like the F20 or Vitera. Hybrid masks may struggle with leak rates at these pressures. You might need BiPAP instead of CPAP at this level.
3. Facial Features and Fit
Different masks accommodate different facial structures:
Prominent Nose or Chin: The F20’s InfinitySeal cushion adapts well to pronounced features. Avoid rigid cushions that create leak points.
Flat Bridge or Asian Facial Features: Hybrid masks like the F30 that don’t rely on the bridge-of-nose seal work better.
Narrow or Small Face: Try the small cushion size for the F20, or look for masks specifically designed with smaller sizing. Standard “small” is often still too large for many women.
Facial Hair: If you have a beard, focus on getting a good seal around your mouth. Consider using mask liners to improve the seal and protect facial hair from pulling.
4. Comfort Features That Actually Matter
Not all comfort features are created equal. Here’s what actually improves long-term compliance:
Magnetic Headgear Clips: Make nightly mask removal for bathroom trips infinitely easier (a major benefit of ResMed masks).
Memory Foam Cushions: Some masks offer memory foam cushions as an alternative to silicone. They’re genuinely more comfortable but require more frequent replacement.
QuietAir or Similar Vent Technology: Reduces noise from 27-30 dB down to 19-21 dB—significant if you have a bed partner.
Minimal Contact Design: Less facial coverage = less irritation, fewer pressure marks (F30, DreamWear).
Forehead-Free Designs: Modern masks skip the forehead strap, reducing claustrophobia (F20, F30).
5. Climate and Environmental Factors
Where you live and sleep affects mask performance:
Dry Climate: Prioritize masks that work well with heated humidification and consider heated tubing to prevent dry mouth.
Humid Climate: The Vitera’s RollFit cushion handles moisture better. Avoid masks with complex vents that clog easily.
Cold Bedroom: Expect more condensation/rainout issues. Heated tubing becomes essential, not optional.
Allergies/Seasonal Congestion: Full-face masks eliminate the mouth breathing caused by a stuffy nose, but you may need to adjust humidification settings seasonally.
CPAP Masks and Chin Straps: Do They Work for Mouth Breathers?
The short answer: sometimes, but usually not.
Many mouth breathers try chin straps as a workaround to keep using nasal masks. While some people find them helpful, the majority of chronic mouth breathers report problems with comfort and effectiveness.
When Chin Straps Might Work
Chin straps can be effective for:
- Occasional mouth breathing (not chronic)
- People whose mouth opens slightly but don’t actively breathe through it
- Those using nasal masks who want insurance against random mouth opening
- Lower pressure settings where small leaks are manageable
Why They Often Fail
For chronic mouth breathers, chin straps fail because:
- They don’t prevent all air leakage from the lips
- Uncomfortable pressure can disrupt sleep
- Jaw clenching causes morning pain (commonly reported)
- Doesn’t address the underlying nasal obstruction
- Compliance is poor (many people stop using them)
Mouth Taping: Controversial, But Some Swear By It
Some people tape their mouths shut instead of using chin straps. This is even more controversial and has serious safety concerns. The risk of suffocation if your nose becomes congested during sleep makes this approach dangerous for most people. Medical professionals generally don’t recommend it.
Bottom Line: If you’re a true chronic mouth breather, skip the accessories and get a proper full-face mask. Your sleep (and your jaw) will thank you.
Common Problems and Solutions for Mouth Breathers Using CPAP
Even with the right mask, mouth breathers face specific challenges. Here’s how to troubleshoot them.
Problem 1: Dry Mouth Despite Full-Face Mask
Possible Causes:
- Humidification set too low
- Mask leaks you haven’t detected
- High pressure forcing air out corners of the mouth
- Mouth still opening inside the mask
Solutions:
- Increase the humidifier setting gradually to 5-7
- Check the mask seal by running CPAP at full pressure while awake
- Try heated tubing to increase moisture delivery
- Ensure mask size fits properly (reseal test during fitting)
Problem 2: Aerophagia (Swallowing Air)
Mouth breathers are more prone to aerophagia—swallowing air that causes bloating, burping, and stomach discomfort.
Solutions:
- Lower pressure if possible (talk to your doctor)
- Switch to BiPAP or auto-adjusting APAP
- Sleep on your side rather than your back
- Avoid eating 2-3 hours before bed
- Consider a smaller mask that doesn’t push against your jaw
Problem 3: Mask Leaks at Mouth Corners
The hardest seal point on full-face masks is often the corners of your mouth, especially if you have facial hair or a distinctive jaw shape.
Solutions:
- Try mask liners to improve the seal
- Ensure proper size (most people oversize their masks)
- Adjust headgear straps—looser is often better
- Consider a memory foam cushion alternative if available for your mask
- Keep facial hair trimmed around the mouth area if you have a beard
Problem 4: Claustrophobia and Anxiety
Full-face masks can trigger anxiety in some users, especially those who’ve never worn one before.
Solutions:
- Start with a hybrid mask (F30 or DreamWear) to ease into full-face
- Practice wearing the mask while awake
- Use the ramp feature to start at a lower pressure
- Read our guide on overcoming CPAP anxiety
- Consider whether a forehead-free design helps (F20, F30)
Problem 5: Red Marks and Skin Irritation
Pressure marks are common with full-face masks, especially if overtightened.
Solutions:
- Loosen straps—mask should be snug, not strangling your face
- Consider a memory foam cushion if available for your mask
- Use mask liners as a barrier between skin and mask
- Try different sleeping positions to reduce pressure
- Clean mask daily to prevent bacterial skin irritation
- Read our guide on preventing CPAP mask marks
CPAP Mask Maintenance for Mouth Breathers
Mouth breathers tend to produce more moisture and oral bacteria in their masks, making proper cleaning even more critical.
Daily Cleaning (Every Morning)
- Disconnect the mask from the hose
- Disassemble the cushion from the frame
- Wash the cushion in warm water with mild soap
- Rinse thoroughly (soap residue causes leaks)
- Air dry completely before next use
- Wipe down the frame with a damp cloth
My routine: I clean my F20 every morning before work. Takes 2 minutes. Non-negotiable. Read my full guide to cleaning CPAP masks.
Weekly Deep Cleaning
- Soak cushion and frame in warm water + mild soap for 15-20 minutes
- Clean headgear in a mesh laundry bag on a gentle cycle
- Inspect all parts for wear, cracks, or degradation
- Check that vent holes aren’t blocked by dried saliva or debris
- Dry everything completely before reassembly
Replacement Schedule
Follow the CPAP replacement schedule for optimal performance:
- Cushion/Pillows: Every 1-2 months (or when seal degrades)
- Frame: Every 6 months (or if cracked/damaged)
- Headgear: Every 6 months (or when elastic stretches)
- Complete Mask: Annually (often covered by insurance)
Mouth breathers should lean toward the more frequent replacement intervals since oral moisture degrades silicone faster.
Cleaning Products to Avoid
Don’t use these on your CPAP mask:
- Harsh detergents or dish soap
- Alcohol-based cleaners
- Bleach or disinfectants
- Ozone CPAP cleaners (FDA warns against these)
- Hot water above 140°F (damages silicone)
Baby shampoo or mild, fragrance-free soap is ideal. That’s it.
Insurance Coverage and Cost Considerations
Most insurance plans, including Medicare, cover CPAP masks for mouth breathers the same as any other mask type.
Insurance Coverage
Medicare Coverage:
- One mask (any type) every 3 months
- Cushion/pillow replacement every month
- Headgear every 6 months
- Must complete initial CPAP compliance period (typically 30-90 days)
Private Insurance:
- Coverage varies significantly by plan
- Most require a prescription from a sleep specialist
- Some cover only specific brands or retailers
- Co-pays range from $0-$50 for masks
My Experience: My insurance covers one new mask every 3 months and monthly cushion replacements. I usually get a full F20 replacement every 6 months and just replace the cushion in between.
Out-of-Pocket Costs
If paying cash or have a high-deductible plan:
- Budget Masks: $80-$120 (older models, basic designs)
- Mid-Range Masks: $130-$180 (Most current full-face)
- Premium Masks: $180-$220 (Latest technology)
- Replacement Cushions: $30-$60
- Headgear: $20-$40
Online retailers often have better prices than durable medical equipment (DME) providers. Just ensure you have a valid prescription.
Insurance and Prescription Requirements
Do You Need a Prescription?
Yes. All CPAP masks require a prescription in the United States, even if you already own a CPAP machine. The prescription must specifically mention CPAP or PAP therapy and should include:
- Diagnosis code (usually G47.33 for obstructive sleep apnea)
- Pressure settings (if applicable)
- Mask type recommendation (though you can usually choose within that category)
- Doctor’s signature and date (within the last 12 months, typically)
Where to Buy CPAP Masks for Mouth Breathers
Sleep Clinics/DME Providers:
- Pros: Face-to-face fitting, insurance billing, expert guidance
- Cons: Higher prices, limited selection, appointment required
Online CPAP Retailers:
- Pros: Lowest prices, widest selection, convenient
- Cons: No fitting assistance, must upload prescription, returns can be tricky
Direct from Manufacturer:
- Pros: Authentic products, direct support
- Cons: Usually the most expensive option
I buy from online retailers for cost savings, but I got my first mask fitted at my sleep clinic. The initial fitting education was valuable even though I buy online now.
My Personal CPAP Mask Experience as a Mouth Breather
Here’s my story—it’s refreshingly simple:
2014-Present: Got diagnosed with severe sleep apnea (AHI 51-60, oxygen dropping to 78%). My sleep clinic prescribed the F20 full-face mask right from the start since I’m a mouth breather. Smart call on their part. First night, my AHI dropped to under 4. I’ve used the same F20 design for over 10 years now, just replacing the cushion every 1-2 months.
I’ve never tried any other mask because I’ve never had a reason to. The F20 works perfectly—why mess with success?
The lesson: Getting the right mask type from the beginning matters. If you’re a chronic mouth breather, a full-face mask isn’t a “backup plan” or something to try after other masks fail. It’s the right starting point.
Special Considerations for Mouth Breathers
Dealing with Seasonal Allergies
I have terrible spring allergies that make mouth breathing worse. During allergy season:
- Increase humidifier setting by 1-2 levels
- Add heated tubing if not already using
- Clean mask more frequently (daily without exception)
- Consider a nasal rinse before bed
- Keep antihistamines consistent
Read more about using CPAP when sick
Mouth Breathing and Teeth Grinding
I’m also a bruxer (teeth grinder), which complicates mask fit. The full-face F20 has enough internal space that I can wear a thin night guard if needed. Tighter hybrid masks don’t have this clearance.
Someone once commented on my TikTok that my teeth “fit together like a jigsaw puzzle” from years of grinding damage. Accurate and mortifying.
Traveling with Full-Face CPAP Masks
Full-face masks are bulkier to pack, but absolutely worth it—I just travel with my F20. Get a good CPAP travel bag with a dedicated mask compartment to protect it during travel.
Read my complete guide to traveling with CPAP
Mouth Breathing and Other Sleep Apnea Treatments
If you’re considering alternatives to CPAP:
- Oral Appliances: Won’t work for mouth breathers—they hold your jaw forward but don’t seal your mouth
- Inspire/Hypoglossal Nerve Stimulation: Addresses mouth breathing at the source but requires surgery
- Sleep Apnea Surgery: Can improve nasal breathing, reducing mouth breathing tendency
Read about alternative sleep apnea treatments
Final Thoughts: Stop Compromising on Mouth Breathing Solutions
After 10+ years of severe sleep apnea, here’s what I know for certain: if you’re a chronic mouth breather, you need a proper full-face or hybrid mask. Period.
Chin straps, mouth tape, and willpower don’t cut it. You’re fighting against decades of breathing patterns and often structural issues like deviated septa or chronic congestion. The path of least resistance is to get a mask designed for your actual breathing pattern.
The ResMed AirFit F20 changed my life. Literally. My AHI went from 51-60 (with oxygen dropping to 78%) down to under 4-5 consistently. I stopped feeling like I’d been hit by a truck every morning. My blood pressure dropped. My brain fog cleared. I stopped falling asleep in meetings.
That first night sleeping with the F20—waking up at 7 AM feeling rested instead of being jolted awake at 3 AM gasping for air—that’s when I knew CPAP therapy could actually work for me. I’ve used the same mask design for over 5 years now because it just works.
If you’re still struggling with your CPAP because you’re mouth breathing through a nasal mask, stop. Get a proper full-face mask. Give it two weeks. The difference will blow your mind.
Your sleep matters. Your health matters. Don’t waste another year being tired because you’re using the wrong equipment.
Frequently Asked Questions
Can you use a nasal CPAP mask if you breathe through your mouth?
Technically, yes, but it’s usually ineffective. The pressurized air escapes through your mouth, reducing therapy effectiveness significantly. Research shows mouth breathers using nasal masks have 60% higher treatment failure rates. Some people succeed with chin straps, but most chronic mouth breathers need a full-face mask.
What’s the difference between a full-face mask and a hybrid mask?
Full-face masks seal from the bridge of your nose to below your mouth, covering everything. Hybrid masks (like the F30) use nasal pillows or under-nose cushions while still covering the mouth. Hybrids have less facial coverage and better field of vision but may seal less reliably than traditional full-face masks.
How do I stop waking up with dry mouth even with a full-face mask?
Increase your CPAP humidifier setting to 5-7. Add heated tubing if you don’t already have it. Check for mask leaks by running your machine at full pressure while awake. Ensure your mask is sized correctly—most people oversize. Consider using distilled water in your humidifier tank.
Will a full-face mask work if I have a beard?
It can, but beards make sealing more challenging. Focus on keeping the area around your mouth trimmed shorter. Use mask liners to improve the seal and reduce pulling. The F20’s InfinitySeal cushion works better than rigid cushions for beards. Read my complete guide for CPAP masks with beards.
How tight should a full-face CPAP mask be?
Snug but not strangling. You should be able to fit one finger between the straps and your head. Over-tightening actually causes more leaks by distorting the cushion shape. The seal comes from the air pressure, not the strap tension. Start looser than you think and only tighten if you detect leaks.
Can mouth breathing cause CPAP therapy to fail completely?
Yes. If you’re using a nasal mask while chronically mouth breathing, the therapy becomes almost useless. The pressurized air meant to keep your airway open escapes, your machine works harder to compensate, creating more leaks, and your AHI stays elevated. Switching to a full-face mask usually drops AHI dramatically.
How often should I replace my full-face CPAP mask?
Replace the cushion every 1-2 months, headgear every 6 months, and the complete mask frame annually. Mouth breathers should lean toward monthly cushion replacement since oral moisture degrades silicone faster. Most insurance covers one complete mask every 3 months and monthly cushion replacements. Read my CPAP replacement schedule guide.
What if I can’t tolerate any full-face mask due to claustrophobia?
Start with a hybrid mask like the F30 or DreamWear that has minimal facial coverage. Practice wearing it while awake, watching TV. Use your machine’s ramp feature to start at a lower pressure. Consider working through CPAP anxiety systematically. If claustrophobia persists, discuss alternative treatments like oral appliances or Inspire therapy with your doctor.
References
- Martins RT, Garbuio S, Moura SM, et al. Mouth breathers can benefit from CPAP use in obstructive sleep apnea syndrome. Dental Press Journal of Orthodontics. 2007;12(4):26-31.
- Bachour A, Maasilta P. Mouth breathing compromises adherence to nasal continuous positive airway pressure therapy. Chest. 2004;126(4):1248-1254. https://pubmed.ncbi.nlm.nih.gov/15486389/
- Epstein LJ, Kristo D, Strollo PJ Jr, et al. Clinical guideline for the evaluation, management and long-term care of obstructive sleep apnea in adults. Journal of Clinical Sleep Medicine. 2009;5(3):263-276. https://pubmed.ncbi.nlm.nih.gov/19960649/
- Koutsourelakis I, Vagiakis E, Roussos C, et al. Obstructive sleep apnoea and oral breathing in patients free of nasal obstruction. European Respiratory Journal. 2006;28(6):1222-1228. https://pubmed.ncbi.nlm.nih.gov/17138806/
- Rowland S, Aiyappan V, Hennessy C, et al. Comparing the efficacy, mask leak, patient adherence, and patient preference of three different CPAP interfaces to treat moderate-severe obstructive sleep apnea. Journal of Clinical Sleep Medicine. 2018;14(1):101-108. https://pubmed.ncbi.nlm.nih.gov/29198310/
- ResMed. AirFit F20 Safety Notice Regarding Magnetic Clips. November 2023. https://document.resmed.com/documents/products/serviceandsupport/mask-magnet-support/Patient_Letter_English_US.pdf
- Kaminska M, Jobin V, Mayer P, et al. The Epworth Sleepiness Scale: self-administration versus administration by the physician, and validation of a French version. Canadian Respiratory Journal. 2010;17(2):27-32. https://pubmed.ncbi.nlm.nih.gov/20422060/
- Pepin JL, Leger P, Veale D, et al. Side effects of nasal continuous positive airway pressure in sleep apnea syndrome. Study of 193 patients in two French sleep centers. Chest. 1995;107(2):375-381. https://pubmed.ncbi.nlm.nih.gov/7842763/
- Borel JC, Gakwaya S, Masse JF, et al. Impact of CPAP interface and mandibular advancement device on upper airway mechanical properties assessed with phrenic nerve stimulation in sleep apnea patients. Respiratory Physiology & Neurobiology. 2012;183(2):170-176. https://pubmed.ncbi.nlm.nih.gov/22750311/
- Oksenberg A, Silverberg DS, Arons E, Radwan H. Positional vs nonpositional obstructive sleep apnea patients: anthropomorphic, nocturnal polysomnographic, and multiple sleep latency test data. Chest. 1997;112(3):629-639. https://pubmed.ncbi.nlm.nih.gov/9315794/
- Ravesloot MJ, van Maanen JP, Dun L, de Vries N. The undervalued potential of positional therapy in position-dependent snoring and obstructive sleep apnea review of the literature. Sleep and Breathing. 2013;17(1):39-49. https://pubmed.ncbi.nlm.nih.gov/22441662/
- McArdle N, Devereux G, Heidarnejad H, et al. Long-term use of CPAP therapy for sleep apnea/hypopnea syndrome. American Journal of Respiratory and Critical Care Medicine. 1999;159(4 Pt 1):1108-1114. https://pubmed.ncbi.nlm.nih.gov/10194153/
- Papsidero MJ, Plante MK, Dyson A. Efficacy and characteristics of a CPAP mask designed specifically for women. Sleep Medicine. 2015;16(5):695-696. https://pubmed.ncbi.nlm.nih.gov/25862119/
- Nigro CA, Dibur E, Malnis S, et al. The influence of gender on symptoms associated with obstructive sleep apnea. Sleep and Breathing. 2018;22(3):683-693. https://pubmed.ncbi.nlm.nih.gov/29147816/
- Massie CA, Hart RW, Peralez K, Richards GN. Effects of humidification on nasal symptoms and compliance in sleep apnea patients using continuous positive airway pressure. Chest. 1999;116(2):403-408. https://pubmed.ncbi.nlm.nih.gov/10453869/
- U.S. Food and Drug Administration. FDA Warns Consumers: Stop Using Unauthorized Ozone-Generating CPAP Cleaners. February 2020. https://www.fda.gov/news-events/press-announcements/fda-warns-consumers-stop-using-unauthorized-ozone-generating-cpap-cleaners
- Centers for Medicare & Medicaid Services. CPAP Coverage Requirements. Medicare.gov. https://www.medicare.gov/coverage/continuous-positive-airway-pressure-cpap-therapy
⚠️ MEDICAL DISCLAIMER This blog provides general information only and is not a substitute for professional medical advice, diagnosis, or treatment. Sleep apnea is a serious condition, and CPAP equipment should be used under proper medical supervision. Always consult your doctor or sleep specialist before starting, stopping, or changing any therapy. I share personal experiences as a CPAP user, not as a medical professional. Individual results vary. For medical guidance, please consult a qualified clinician or the American Academy of Sleep Medicine (aasm.org).