CPAP Sleep Study – What to Expect from a Polysomnography Test

I avoided school camp as a kid. Not because I didn’t want to go, but because I knew what would happen. I’d keep everyone awake with my snoring, someone would complain, and I’d spend the rest of the trip embarrassed about it. Worst case, I would have a boot thrown in my face at 2 am. At the time, I just thought I was a loud sleeper. I had no idea there was something genuinely wrong with me.
That something turned out to be obstructive sleep apnea at a severe level, and it took a sleep study to finally put a number on it. Sixty apneas an hour. Once every single minute. My airway was collapsing so frequently through the night that I was never getting into proper restorative sleep. My heart was under strain, I hadn’t consented to. And I was walking around for years thinking the exhaustion was just… life. That’s what blows my mind looking back.
My sleep study changed everything. If you’re wondering whether you need one, or you’ve been referred for one and you’re not sure what to expect, this is the post I wish I’d had before mine.
What a Sleep Study Actually Is
The formal name is polysomnography, and I’ll use PSG as shorthand because nobody in real life says polysomnography twice in a row. It’s an overnight test done in a sleep lab, where you’re monitored while you sleep with sensors tracking pretty much everything your body is doing. Brain activity, eye movement, heart rhythm, oxygen levels, breathing effort, and muscle activity in your legs and chest. They also run a microphone and video camera, so any gasping, snoring, or movement gets captured too.
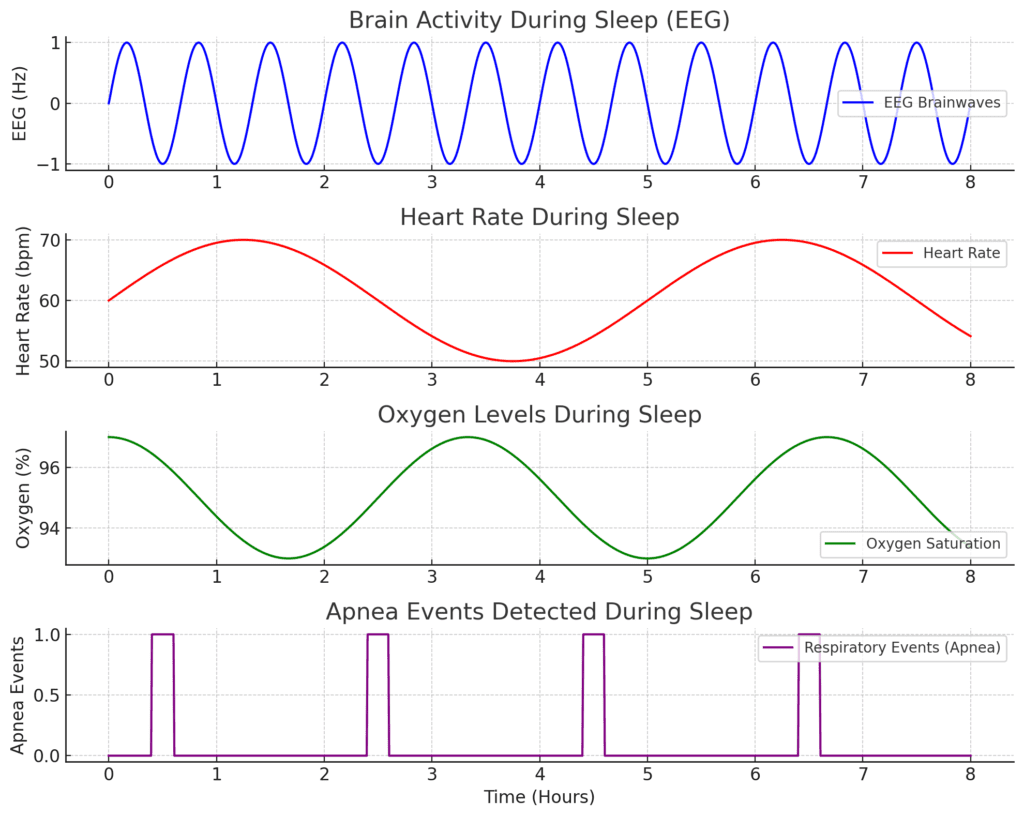
The idea is to build a complete picture of what’s happening while you sleep, because most of what sleep apnea does to you happens invisibly. You’re not awake for any of it. You don’t know your airway is collapsing. You don’t know your blood oxygen is dropping. You wake up feeling like you’ve been hit by a bus, and you genuinely don’t understand why, because as far as you know, you slept eight hours.
A PSG isn’t the same as a home sleep test, which only captures a narrower set of data and doesn’t monitor brain activity. An in-lab study is the most comprehensive option and is particularly useful for more complex or severe cases. I’ll come back to the home test option a bit later.
What Happens on the Night
You arrive a couple of hours before you’d normally go to sleep. The room doesn’t look like a hospital ward, which I think surprises a lot of people. It’s more like a basic hotel room with a comfortable bed, a bit of privacy, and a generally quiet atmosphere. The clinical element is the technician who spends time attaching sensors to your scalp, face, chest, and legs before you try to sleep.
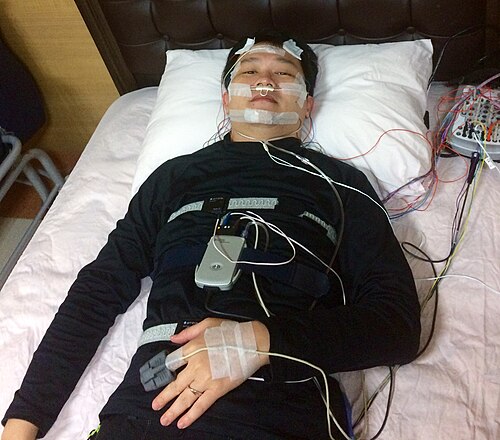
I won’t pretend it’s completely comfortable. You’re essentially wired up to a monitoring system with electrodes on your head and straps around your chest. For the first little while, you’re very aware of it all. But most people fall asleep faster than they expect, partly because anyone heading into a sleep study is usually already chronically sleep-deprived. The technician watches everything from a separate room and can communicate with you through an intercom if needed.
One thing worth knowing is that if your study strongly suggests moderate or severe sleep apnea during the first half of the night, the technician may convert your test into a split-night study. That means the second half of the night becomes what’s called a CPAP titration, where they fit you with a mask and try different pressure levels until they find the setting that eliminates your apneas. My first night on CPAP happened exactly this way. I woke up the next morning feeling more alert than I had in years. That single night was enough to convince me that therapy was going to work.
Reading Your Results
When you get your results back, they can look like a wall of abbreviations and numbers. The one that matters most for most people is the AHI, which stands for Apnea-Hypopnea Index. This is simply the number of breathing interruptions recorded per hour of sleep. Under five is considered normal. Five to fifteen is mild. Fifteen to thirty is moderate. Above thirty is severe.

Mine was 51. The technician pointed it out almost carefully, like they were bracing for a reaction. One apnea every minute of sleep, all night long, for years. It explained the sore throats I’d been waking up with, the headaches and migraines that had been getting more frequent, and the brain fog I’d been putting down to stress. It also explained the concern my doctor had raised about the pressure it was putting on my heart.
Beyond the AHI, a PSG also shows your oxygen desaturation index, which tracks how often your blood oxygen is dropping below healthy levels during the night. It shows your sleep staging, meaning how much time you actually spent in light sleep versus deep sleep versus REM. And it tracks arousals, which are the moments your brain briefly wakes itself up to restart your breathing, even when you don’t consciously register it. In my case, I was stuck in light sleep almost the entire night because my brain kept pulling me back from deeper stages every time my airway collapsed.
Understanding sleep stages matters here. A normal night cycles through light sleep, deep sleep, and REM sleep several times over, and each stage does something different for you. Deep sleep is when your body does its physical repair work. REM sleep is where memory consolidation and emotional processing happen. When apnea keeps fragmenting your sleep all night, you’re robbed of both, and it shows in how you feel and function during the day.
What the Study Can Also Detect
The primary reason most people end up in a sleep lab is suspected sleep apnea, but a PSG can pick up other things too. Periodic limb movement disorder, where your legs jerk involuntarily through the night, shows up in the muscle monitoring data. REM behaviour disorder, where people physically act out their dreams, gets captured on the video and EEG. Narcolepsy requires a follow-up daytime test called the Multiple Sleep Latency Test, but the overnight PSG is usually part of the diagnostic process. Central sleep apnea, which is a different condition to obstructive sleep apnea and requires different treatment, also gets identified through the overnight data.
This is one of the big advantages of the in-lab study over a home test. You can’t detect all of these things with a device you strap to your wrist at home.
PSG vs the Home Sleep Test
Speaking of which, it’s worth comparing the two options honestly, because cost is a real factor and the home test is significantly cheaper. An in-lab PSG runs in the range of one to three thousand pounds or dollars before insurance. A home sleep apnea test typically costs a fraction of that.
The home test is a simpler device you wear overnight in your own bed, usually measuring your breathing, oxygen saturation, and heart rate. It doesn’t monitor brain activity and it can’t tell you your sleep stages or detect the full range of sleep disorders. For straightforward cases of suspected obstructive sleep apnea, a home test is often sufficient to get a diagnosis and a CPAP prescription. For anything more complex, or if the home test comes back inconclusive, an in-lab study gives you the complete picture.
I’d recommend reading my full post on the at-home sleep apnea test if you’re weighing up your options. Depending on where you live and what your healthcare system covers, the home test might be your most practical first step.
When You Should Probably Get Tested
My partner is the one who finally pushed me to do something. She’d noticed I was stopping breathing in my sleep, which is terrifying to watch from the outside even if you’re completely oblivious to it from the inside. I’m genuinely grateful she said something, because I’d been explaining away the symptoms for so long that I’d stopped questioning them.
If you’re snoring heavily and people near you have mentioned it, that’s a reason to get checked. If you wake up gasping or choking, that’s a reason. If you’re getting seven to nine hours of sleep and still waking up exhausted, if you’re getting morning headaches regularly, if you’re struggling with concentration and memory in ways that feel out of proportion to your stress levels, those are all reasons. High blood pressure and certain heart arrhythmias are also associated with untreated sleep apnea, so if you’re managing either of those conditions, it’s worth raising with your doctor.
You don’t need to tick every box. I’d had years of symptoms and still kept dismissing them. If something feels off about your sleep, it’s worth investigating.
What to Bring and How to Prepare
Treat it like a one-night hotel stay. Bring comfortable pyjamas or whatever you normally sleep in, your own pillow if that helps you settle, toiletries, something to wind down with in the hour before you try to sleep, and a change of clothes for the morning. Avoid caffeine after early afternoon on the day of the test, and skip any naps that day. You want to arrive genuinely tired rather than artificially alert.
If the study is being done as part of a titration and you already have a preferred mask style from a previous CPAP trial, mention that to the technician when you arrive. Most labs carry a range of options, including nasal pillows, nasal masks, and full face masks, and they’ll want you to be as comfortable as possible.
What Happens If the Results Are Inconclusive
It does happen. You might not sleep long enough, or your apnea might not show up on a particular night with the same frequency it normally does. If your results are borderline, your doctor might repeat the PSG on another occasion, try a home sleep test for comparison, or look at other explanations for your symptoms. Sleep is variable, and one night doesn’t always capture the whole picture. It’s worth being patient with the process rather than writing it off if the first study doesn’t give you a clear answer.
What Comes After
If the study confirms sleep apnea, your sleep specialist will talk you through the options. For most people with obstructive sleep apnea, that means CPAP therapy. In some cases it might also involve advice around weight loss, sleep position, or other lifestyle factors. If there’s a structural component, like a deviated septum, that might be part of the conversation too.
For me, getting started on CPAP was quick because my titration happened on the same night as my diagnostic study. The change was immediate and significant. That sounds like something you’d write as a tagline, but it’s genuinely what happened. I woke up alert. My brain worked. The migraines became less frequent. The fog started lifting. After years of explaining all of that away, getting an actual answer and an actual treatment felt almost surreal.
If you’re sitting on the fence about whether to pursue a sleep study, my honest take is that it’s worth doing sooner rather than later. The longer sleep apnea goes untreated, the more cumulative damage it does. Getting diagnosed doesn’t commit you to anything; it just gives you information. And in my experience, that information changes things.
⚠️ MEDICAL DISCLAIMER This blog provides general information only and is not a substitute for professional medical advice, diagnosis, or treatment. Sleep apnea is a serious condition, and CPAP equipment should be used under proper medical supervision. Always consult your doctor or sleep specialist before starting, stopping, or changing any therapy. I share personal experiences as a CPAP user, not as a medical professional. Individual results vary. For medical guidance, please consult a qualified clinician or the American Academy of Sleep Medicine (aasm.org).