What Does CPAP Stand For? A Guide From 10+ Years Experience

I’ll never forget a night in a Melbourne hostel when my bunkmate threw a pillow at my face at three in the morning. “Mate, you stopped breathing for like thirty seconds,” he said, looking genuinely shaken. “I thought you were dying.”
I laughed it off. Told him I was just a heavy sleeper. But the look on his face stayed with me, and when I got home I finally made the appointment I’d been putting off for years. The sleep study results were not what I’d expected. My AHI was 58, meaning I was waking up 58 times every hour as my body gasped for air. My blood oxygen was dropping to 78% during the night. My sleep specialist told me, without softening it, that my brain was being starved of oxygen for hours every night and my heart was under serious strain.
That was the first time I heard the term CPAP therapy. I had absolutely no idea what it meant, and the alphabet soup of medical acronyms surrounding it made everything feel more overwhelming than it needed to be. So let me explain it in plain English the way I wish someone had explained it to me.
What CPAP Actually Stands For
CPAP stands for Continuous Positive Airway Pressure. Each word in that name is doing real work, so it’s worth unpacking them.
Continuous means the machine delivers air pressure constantly and steadily throughout the night, not just when it detects a problem. Positive Airway Pressure means the air being delivered is at a pressure slightly above atmospheric, which is what keeps your airway propped open. And airway is the key word, because that’s the whole point. In obstructive sleep apnea, the soft tissues in your throat relax during sleep and collapse inward, blocking airflow. Your brain notices you’ve stopped breathing, jolts you into a lighter sleep state just enough to restore muscle tone, your airway reopens, and the cycle starts again. Dozens or hundreds of times a night, depending on severity. CPAP interrupts that cycle by maintaining enough pressure in your airway that it physically cannot collapse.
When I first saw a CPAP mask, I genuinely thought it looked like something from a science fiction film. The idea that I’d sleep comfortably with that strapped to my face seemed absurd. But here’s what put it in perspective: without treatment, my brain was being wrenched out of deep sleep 58 times every single hour. With CPAP, that number dropped to under 5. The mask suddenly seemed a lot more reasonable.
How the Machine Works in Practice
The setup is simpler than it looks. A CPAP machine pulls in room air, filters it, pressurises it to your prescribed level, and delivers it through a hose to a mask that seals against your face. The air pressure is measured in centimetres of water, written as cm H₂O. Most people with obstructive sleep apnea are prescribed somewhere between 6 and 15 cm H₂O, though some need higher. Mine is set at 14.
Modern machines are remarkably quiet, nothing like the loud mechanical noise people sometimes imagine. My ResMed AirSense 10 is closer to a gentle hum than anything disruptive. They also come with a built-in humidifier, which matters a lot in practice. Pressurised air without humidity dries out your nose and throat quickly, and without the humidifier running properly, you’ll wake up with a very sore, dry mouth. I run mine at level 4 and always use distilled water in the chamber rather than tap water, which leaves mineral deposits over time.
Most machines also have a ramp function, which starts the pressure lower when you first put the mask on and gradually increases it to your prescribed level over ten or twenty minutes as you fall asleep. I used this every night for the first year and still do. It makes the transition into sleep much more comfortable than being hit with full pressure immediately. The how a CPAP machine works post goes into more detail on the mechanics if you want a deeper look.
The Other Acronyms You’ll Come Across
Once you’re in the sleep apnea world you’ll quickly encounter APAP, BiPAP, and a few others. They’re all variations on the same basic principle but work differently, and knowing what they mean makes it easier to have an informed conversation with your sleep specialist.
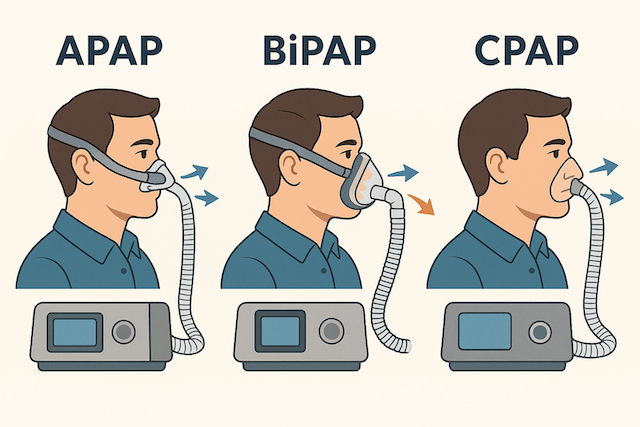
APAP stands for Automatic Positive Airway Pressure, sometimes called Auto-CPAP. Rather than delivering one fixed pressure all night, an APAP machine uses algorithms to monitor your breathing continuously and adjusts the pressure up or down in real time based on what your airway needs at any given moment. When you roll onto your back, your airway is more prone to collapsing and the machine increases pressure. When you’re sleeping well on your side, it backs off. For people whose sleep apnea severity varies a lot across the night or between nights, an APAP can deliver more comfortable therapy than a fixed-pressure machine because it’s not pushing unnecessary pressure when you don’t need it. I have a dedicated post on how APAP works if this is the route you’re considering.
BiPAP stands for Bilevel Positive Airway Pressure, and the key difference is that it uses two separate pressure settings rather than one. There’s a higher pressure for when you breathe in and a lower pressure for when you breathe out. The reason this matters is that some people, particularly those who need higher overall pressures, find it genuinely difficult to exhale against constant pressure. With BiPAP, that exhalation pressure drops, making breathing feel far more natural. I haven’t needed to switch from standard CPAP myself, but I tested a BiPAP during a titration study once and the difference in how breathing felt was striking. If you’re struggling to exhale against your CPAP pressure, it’s absolutely worth raising with your doctor. My full CPAP vs BiPAP comparison explains the trade-offs in detail.
ASV, or Adaptive Servo-Ventilation, is a more specialised machine designed for complex sleep apnea, which is a combination of obstructive and central apnea. It goes beyond what an APAP does by monitoring and responding to your breathing pattern on a breath-by-breath basis. Most people with straightforward obstructive sleep apnea won’t need this, but it’s worth knowing exists if your situation is more complicated.
The umbrella term for all of these is PAP therapy, which just means Positive Airway Pressure and covers any treatment using pressurised air to manage sleep-disordered breathing.
The Three Parts of Your Setup
Whatever machine type you end up with, every CPAP setup has three main components and each one matters.
The machine itself is the pressure generator. Beyond the core function, modern machines track your data automatically, including your AHI each night, your mask leak rate, and how many hours you used the therapy. That data gets wirelessly sent to your sleep team and is also accessible to you. I check mine regularly and it gives me a lot of reassurance that the therapy is actually doing what it should be doing. My guide to interpreting CPAP data explains what the numbers mean if you’re new to reading it.
The hose connects the machine to the mask and is where rainout can become an issue. Rainout is when warm humid air from the machine cools down in the hose during colder nights and condenses into water droplets that travel toward your face. Getting heated tubing eliminates this almost entirely by keeping the air temperature consistent along the whole length of the hose. It’s one of the first upgrades I’d recommend.
The mask is where most of the personalisation happens, and it’s also where most people struggle initially. There are three main styles: full face masks that cover both your nose and mouth, nasal masks that cover just your nose, and nasal pillows that seal directly at your nostrils. I use a full face mask because I’m a mouth breather, and without covering my mouth the pressurised air would simply escape that way. If you breathe through your nose, a nasal mask or nasal pillows might suit you better. I tried several masks before finding one that sealed well and felt comfortable. The how to choose a CPAP mask post walks through the decision in more detail.
What to Expect When You’re Starting Out
The adjustment period is real and it’s worth being honest about it. Wearing a mask strapped to your face while you sleep is an unusual sensation, and it takes most people a few weeks to stop noticing it. Some people take longer. The first thing I’d say is that struggling in the early weeks is completely normal and doesn’t mean the therapy isn’t going to work for you.
The ramp function helps a lot with those early nights. So does wearing the mask for short periods during the day while you’re awake and relaxed, watching something on television or reading. It helps your brain stop associating the mask purely with the stress of trying to sleep in it. My post on overcoming CPAP anxiety goes into more practical strategies if this is the part you’re finding hard.
The common early problems, mask leaks, dry mouth, and rainout, all have straightforward fixes once you know what’s causing them. I’ve written a dedicated CPAP troubleshooting guide covering all of the most common issues and what actually resolves them. Most problems trace back to either a mask that isn’t fitting well or a humidifier that isn’t set correctly for your environment.
One thing that genuinely surprised me about my first proper night on CPAP, which happened during my titration study in the sleep lab, was how immediately different I felt the next morning. I woke up alert in a way I hadn’t experienced in years. That one night was enough to convince me the therapy was going to work, and it made tolerating the adjustment period much easier because I knew what was on the other side of it.
Why It Matters Beyond Just Sleeping Better
Sleep apnea does damage that goes well beyond feeling tired. Before my diagnosis, I was dealing with regular morning headaches, brain fog that made concentrating on anything difficult, and worsening cardiovascular numbers that my doctor couldn’t fully explain. The repeated oxygen drops through the night put significant strain on the heart and over time increase the risk of high blood pressure, stroke, and other serious complications. My blood pressure was sitting at 145/90 before I started CPAP therapy. It normalised within a few months of consistent use.
The brain fog clearing was the thing that surprised me most. I’d become so accustomed to it that I’d stopped recognising it as a symptom. It felt like normal adult tiredness. It wasn’t. Within two weeks of starting therapy it was noticeably better, and within a month I felt like a different person. If you want more on the longer-term picture, my post on whether CPAP increases life expectancy covers the evidence in plain terms.
The Simple Version
CPAP stands for Continuous Positive Airway Pressure. It works by delivering a constant, pressurised stream of air through a mask that keeps your airway from collapsing during sleep. It’s the most effective treatment available for obstructive sleep apnea, and for most people with a moderate to severe diagnosis, it’s where treatment starts.
The early weeks involve some adjustment. The acronyms are confusing at first. The equipment looks more intimidating than it is. But the gap between how I felt before treatment and how I feel now, over a decade later, is not something I could adequately describe in a few sentences. Getting diagnosed was the most important thing I ever did for my health, and starting therapy was the most important thing I ever did with that diagnosis.
If you’re at the beginning of this journey and feeling overwhelmed by it, that’s completely understandable. It gets easier quickly, and the effort is absolutely worth it.
⚠️ MEDICAL DISCLAIMER This blog provides general information only and is not a substitute for professional medical advice, diagnosis, or treatment. Sleep apnea is a serious condition, and CPAP equipment should be used under proper medical supervision. Always consult your doctor or sleep specialist before starting, stopping, or changing any therapy. I share personal experiences as a CPAP user, not as a medical professional. Individual results vary. For medical guidance, please consult a qualified clinician or the American Academy of Sleep Medicine (aasm.org).





