Best CPAP Mask for Stomach Sleepers: Top 4 Ranked for 2026
“This post contains affiliate links. I may earn a commission if you buy through these links, at no extra cost to you. Read my Disclaimer for more details.”
Here’s something I’ve learned after a decade in CPAP communities: stomach sleepers face one of the toughest challenges in sleep apnea therapy. I can’t count how many times I’ve seen someone post in frustration, “I’ve tried three different masks and I still wake up with my face pressed into the pillow and air hissing everywhere.”

I’ll be honest upfront—I’m not a stomach sleeper myself. I use the ResMed AirFit F20 full-face mask, and sleeping on my stomach with that thing would be like trying to nap on a dinner plate. But over 10+ years of helping others navigate CPAP therapy through Reddit, Facebook groups, and my blog, I’ve developed deep expertise in what actually works for stomach sleepers.
This article draws from countless conversations with real CPAP users, peer-reviewed research on sleep positioning and therapy compliance, and my understanding of mask engineering from years of studying this equipment. If you’re one of the rare 7% who sleep on your stomach, this guide will help you find a mask that actually stays put.
The 4 Best CPAP Masks for Stomach Sleepers (Ranked)
After analyzing user reviews from CPAP forums and Facebook groups, combined with my understanding of mask engineering, here are the top masks that actually work for stomach sleepers:
🥇 1. ResMed AirFit P30i – Best Overall for Stomach Sleepers

The AirFit P30i solves the fundamental problem of stomach sleeping with its innovative top-of-head hose connection. I’ve seen more stomach sleepers succeed with this mask than any other.
Why it dominates for stomach sleepers:
The top-mounted tubing means nothing pulls on your face when you turn. The hose literally comes off the crown of your head, so pillow contact doesn’t create tension on the mask seal. The nasal pillow design has minimal facial contact—just two small cushions that sit in your nostrils.
The SpringFit frame is genius for active sleepers. It flexes and moves with you rather than fighting against your movements. I’ve had multiple people tell me this was the first mask that “disappeared” during sleep.
Technical specifications:
- Nasal pillow mask with three cushion sizes (small, medium, large)
- Top-of-head 360° swivel connection
- QuietAir vent technology (diffused exhalation for partner comfort)
- Compatible with all ResMed CPAP and BiPAP machines
- Weight: 1.6 oz (one of the lightest masks available)
Best for: Pure stomach sleepers who don’t mouth breathe. If you’re nasal-only, this is your first choice.
Limitations: Not suitable for mouth breathers without adding a chin strap. Also struggles at very high pressure settings (above 15 cm H2O).
Community feedback: In Reddit’s r/CPAP community, the P30i consistently gets mentioned as the “game-changer” for stomach sleepers. One user wrote: “I went through four masks in two months before finding the P30i. Finally sleeping through the night.”
🥈 2. ResMed AirTouch N30i – Most Comfortable

The N30i takes everything great about the P30i and swaps silicone nasal pillows for a memory foam nasal cradle. If the idea of inserts in your nostrils makes you uncomfortable, this is your alternative.
Why it earns silver:
The memory foam cushion sits under your nose rather than in it, creating an incredibly gentle seal. People with sensitive skin or nostril irritation often find this design more tolerable for long-term use. The top-of-head tubing configuration matches the P30i, giving you the same freedom of movement.
Technical specifications:
- Nasal cradle (under-nose) design with memory foam cushion
- Top-of-head QuickFit™ auto-adjusting headgear
- UltraSoft™ memory foam that adapts to facial contours
- Three cushion sizes available
- 100% washable except cushion (cushion is disposable)
Best for: Sensitive skin, nostril irritation, or anyone who finds nasal pillows uncomfortable but needs a low-profile mask.
Limitations: The memory foam cushion can’t be washed and needs replacement every 30 days, which increases long-term costs. Some users report the cushion compresses over time, reducing seal effectiveness after 3-4 weeks.
Personal note: I’ve had several people with deviated septums tell me the N30i worked where nasal pillows failed. The broader contact area distributes pressure more evenly.
🥉 3. Philips Respironics DreamWear Nasal CPAP Mask – Best Alternative to ResMed

If ResMed masks don’t work for you (facial shape, sizing, or preference), the DreamWear is your next stop. It pioneered the top-of-head design concept and remains excellent for stomach sleepers.
Why it gets bronze:
The DreamWear’s hollow frame design is brilliant—air flows through the frame itself to nasal cushions under your nose. This eliminates the traditional front-connection tubing problem entirely. The under-nose cushion means you can sleep with your mouth open without breaking the seal (though you’ll still need proper CPAP pressure settings for this to work).
Technical specifications:
- Under-nose nasal cushion design
- Hollow frame with integrated airflow pathway
- Top-of-head 360° swivel elbow
- Fabric frame wraps (available separately) for added comfort
- Modular design allows switching between nasal and full-face cushions
Best for: People who prefer Philips equipment ecosystems, those who find ResMed cushions don’t fit their facial structure, or anyone wanting the option to upgrade to full-face cushions later.
Limitations: The frame can feel bulkier than the minimal P30i design. Some users report seal issues at higher pressures (above 12 cm H2O). The cushion sits under the nose, which some people find less secure than nasal pillows.
Compatibility note: Works with all standard 22mm CPAP tubing, but pairs especially well with Philips DreamStation machines for integrated data tracking through the DreamMapper app.
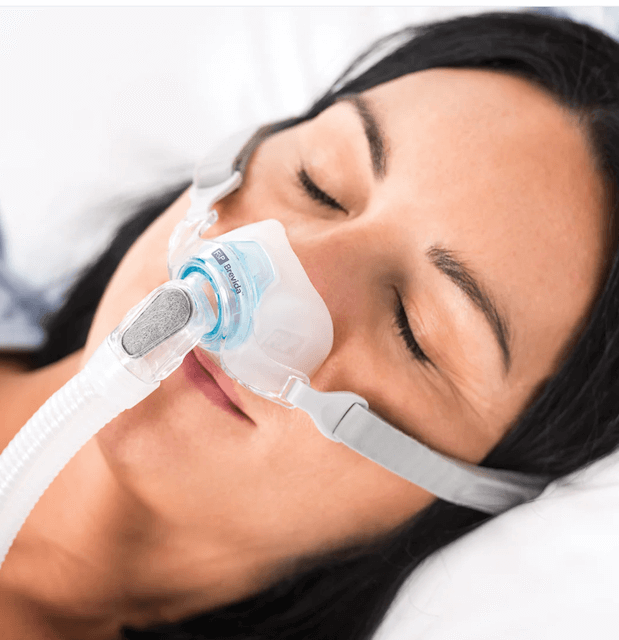
⭐ 4. ResMed AirFit F30i – Best for Mouth-Breathing Stomach Sleepers

I know this lady is sleeping on her back, but this full face mask is also great for stomach sleepers.
This is the holy grail if you sleep on your stomach AND breathe through your mouth: a full-face mask with top-of-head tubing. I know it sounds impossible, but ResMed engineered it.
Why it makes the list:
Traditional full-face masks are disasters for stomach sleepers—they’re bulky, press into pillows, and create massive leak issues. The F30i solves this with its under-nose full-face cushion design. Instead of covering your entire nose like the traditional F20, it sits under your nostrils and over your mouth.
The top-of-head QuickFit™ headgear eliminates the tubing-pull problem. The lack of forehead support actually becomes an advantage here—there’s no rigid frame to dig into your pillow.
Technical specifications:
- Under-nose full-face cushion (covers mouth, sits under nose)
- Top-of-head QuickFit™ auto-adjusting headgear
- Magnetic clips for easy attachment/detachment
- UltraCompact cushion design minimizes facial coverage
- Three cushion sizes available
Best for: Mouth breathers, chronic nasal congestion, anyone with nasal obstruction, or stomach sleepers who need higher CPAP pressures.
Limitations: Still bulkier than nasal options. Takes adjustment time—most users report needing 5-7 nights to adapt. Not as comfortable for pure side sleeping as it is for stomach sleeping.
Real-world feedback: I’ve corresponded with several people who thought stomach sleeping with a full-face mask was impossible until they tried the F30i. One user described it as “the only full-face mask I can actually sleep in face-down.”
Why Stomach Sleeping Makes CPAP So Challenging
Let’s talk about what makes stomach sleeping uniquely difficult for CPAP therapy—because understanding the problem helps you solve it.
The Physics of Face-Down Sleep
When you sleep on your stomach, your face presses directly into your pillow. This creates several mechanical problems that don’t exist for back or side sleepers:
Mask displacement from pillow pressure. Research shows that stomach sleeping is the least common sleep position, affecting only about 7% of adults, but it creates the highest rate of mask leaks and displacement. Your pillow essentially pushes against your mask from multiple angles, breaking the seal that keeps therapy effective.
Forced neck rotation. Unless you’ve mastered sleeping with your face straight down (please don’t—you need to breathe), stomach sleeping requires turning your head to one side. This rotation can pull on your headgear straps, shifting the mask position throughout the night.
Tubing entanglement. Traditional front-connected CPAP hoses become anchoring points when you’re face down. The hose pulls, you move, the mask shifts—it’s a recipe for frustration and air leaks.
The Medical Complications
Beyond the mechanical issues, stomach sleeping interacts with sleep apnea in complex ways:
Some research suggests stomach sleeping may actually improve central sleep apnea by preventing the tongue from falling backward and blocking the airway. However, for the far more common obstructive sleep apnea, stomach sleeping can aggravate neck and spine problems while making CPAP therapy significantly harder to maintain.
The relationship between sleep position and apnea severity is well-documented in sleep medicine literature. Studies show that sleep position affects airway collapse patterns, with back sleeping being particularly problematic for most OSA patients. But stomach sleeping, while potentially helpful for airway mechanics, creates such significant mask compliance issues that its theoretical benefits are often negated by poor therapy adherence.
The Compliance Crisis
Here’s the harsh reality: up to 50% of CPAP users don’t stick with their therapy, and mask discomfort is one of the leading causes. For stomach sleepers, that number is likely higher because finding a compatible mask is genuinely harder.
When patients abandon CPAP therapy due to mask issues, they’re left with untreated sleep apnea, which increases risks for cardiovascular disease, stroke, diabetes, and other serious health conditions. This is why finding the right mask isn’t just about comfort—it’s about your long-term health.
What Makes a CPAP Mask Actually Work for Stomach Sleepers?
Understanding these design features will help you evaluate any mask, not just the ones I’ve recommended:
1. Top-of-Head Hose Connection (Non-Negotiable)
This is the single most important feature for stomach sleepers. Traditional front-connected hoses create an anchor point that gets compressed when you press your face into the pillow. That compression pulls the mask, breaks the seal, and wakes you up with air hissing across your face.
Top-of-head connections eliminate this problem entirely. The hose rises from the crown of your head, meaning pillow contact doesn’t create pulling forces on your mask.
2. Minimal Facial Contact Points
The less mask surface touching your face, the fewer pressure points when you’re face-down. Nasal pillow designs win here—they only contact the rim of your nostrils and your headgear strap areas.
Nasal masks cover more surface area, which can work for some stomach sleepers if the cushion is soft enough to compress without losing seal. Full-face masks traditionally struggle here, which is why the F30i’s under-nose design is revolutionary.
3. Flexible Frame Engineering
Rigid frames are your enemy. When you move during sleep, a rigid frame maintains its shape and breaks seal. Flexible frames like the P30i’s SpringFit design move with you, maintaining seal integrity through positional changes.
The DreamWear takes a different approach with its fabric frame, which distributes forces across the entire frame structure rather than concentrating them at seal points.
4. Quiet Exhalation Vents
This matters more for stomach sleepers than you might think. When your mask is pressed against a pillow, poorly designed vents can amplify noise like a speaker cone. The P30i’s QuietAir venting and similar diffused vent systems redirect exhaled air away from your face and dampen the sound.
Your bed partner will thank you for this feature—and you’ll sleep better without the whooshing sound six inches from your ears.
5. 360° Swivel Connections
Look for masks where the hose connection swivels freely. This prevents tubing torque from transferring to your mask when you rotate during sleep. ResMed’s ball-and-socket swivel design is particularly effective here.
Beyond Masks: Complete Setup for Stomach-Sleeping CPAP Success
The mask is crucial, but it’s only part of the equation. Here’s what else matters:
CPAP Pillows Make a Massive Difference
I cannot overstate this enough: get a CPAP-specific pillow. These aren’t marketing gimmicks—they’re ergonomically designed with cutouts that accommodate your mask and reduce pressure points.
Standard pillows force you to compress your mask against a flat surface. CPAP pillows create space for your mask to exist without constant pressure. Many have side cutouts that are perfect for stomach sleepers who need to rotate their head to one side.
Personal recommendation: The Hero CPAP Pillow has worked well for several people I’ve advised. The center cutout accommodates both nasal and full-face masks for stomach positioning.
Hose Management Systems
A hose holder or suspension system prevents your tubing from pulling on your mask when you move. For stomach sleepers with top-of-head connections, this is less critical than for front-connected masks, but it still helps.
I recommend either a hose lift that mounts to your headboard or a simple hose clip system. The goal is slack management—you want enough hose freedom to move without creating tension that pulls your mask.
Humidity Settings Matter More Than You Think
CPAP humidifiers prevent dryness, but they can also affect mask seal. If your humidifier runs too hot, you risk CPAP rainout—condensation that pools in your mask and breaks the seal.
For stomach sleepers, I recommend starting with medium humidity (level 3 out of 5 on most machines) and adjusting based on comfort. Consider heated tubing if you’re getting condensation issues—it maintains a consistent temperature and prevents water buildup.
Pre-Bedtime Facial Prep
This seems minor, but it makes a real difference: wash your face before bed. Skin oils break mask seals, and stomach sleepers can’t afford ANY seal compromise. A quick cleanse with mild soap removes oils and improves cushion adhesion.
Similarly, clean your mask daily. Dirty cushions lose their sealing properties faster, and stomach sleepers need every advantage for maintaining seal integrity.
Alternative Approaches: Should You Try to Change Sleep Positions?
Here’s an uncomfortable truth: stomach sleeping is genuinely challenging for CPAP therapy, and some sleep specialists recommend training yourself to sleep differently.
The Case for Side Sleeping
Side sleeping is considered optimal for sleep apnea because it prevents gravity from collapsing your airway the way back sleeping does. It also accommodates CPAP masks much better than stomach sleeping.
If you’re willing to try positional therapy, the tennis ball technique actually works: wear a pocketed t-shirt backward to bed with a tennis ball in the back pocket. When you try to roll onto your back or stomach, the discomfort prompts you to return to side sleeping.
Modern alternatives include positional therapy devices like vibrating alarms that detect when you’re on your back and gently prompt you to shift positions. Some CPAP users report successfully retraining their sleep position over 2-3 weeks.
When Stomach Sleeping Is Non-Negotiable
Some people simply cannot sleep any other way. Chronic back pain, pregnancy recovery, spinal conditions, or just deeply ingrained habits can make position changes impossible or unhealthy.
If that’s you, don’t force it. Focus instead on optimizing your CPAP setup for stomach sleeping. A compatible mask with proper accessories will deliver effective therapy—it just requires more attention to equipment selection.
Troubleshooting Common Stomach-Sleeper CPAP Problems
Even with the right mask, you might encounter these issues:
Problem: Mask Still Leaks When Face-Down
Solutions:
- Verify you have the correct cushion size—most masks include multiple sizes
- Check headgear tension—it should be snug but not tight (you shouldn’t feel pressure points)
- Try mask liners (like RemZzzs) to improve seal and reduce skin irritation
- Ensure your CPAP pillow provides adequate mask clearance
If leaks persist, your mask might not be compatible with your facial structure. Consider trying a different design from my recommendations above.
Problem: Neck or Shoulder Pain
Stomach sleeping inherently stresses your cervical spine. CPAP equipment can worsen this if your pillow forces awkward head angles.
Solutions:
- Invest in a proper CPAP pillow designed for stomach sleepers
- Ensure your regular pillow isn’t too thick (over-extension strains your neck)
- Consider a physical therapy evaluation if pain persists—sleep position might be causing structural damage beyond CPAP issues
Problem: Dry Mouth Despite Nasal Mask
This indicates mouth breathing during sleep, which breaks the therapy circuit. Your CPAP delivers pressure to your nose, but if your mouth opens, air escapes before reaching your lungs.
Solutions:
- Try a chin strap to keep your mouth closed
- Increase humidifier settings to reduce mucosal drying
- If chin straps don’t work, switch to the AirFit F30i or another full-face option
CPAP dry mouth is common and manageable, but it requires addressing the root cause: air escape.
Problem: Headgear Marks or Skin Irritation
Stomach sleeping can increase headgear pressure against your pillow, which transfers to your skin.
Solutions:
- Try CPAP strap covers or mask liners
- Ensure headgear isn’t over-tightened (common mistake when fighting leaks)
- Adjust your sleeping position slightly—even a 15-degree angle shift can relieve pressure points
- Consider masks with fabric headgear instead of traditional elastic straps
Some people develop CPAP dermatitis from prolonged contact with mask materials. If you see redness, rashes, or persistent irritation, consult your doctor.
Problem: Can’t Fall Asleep with Mask On
This is more psychological than mechanical, but it’s real. Stomach sleepers often report feeling “trapped” by their mask.
Solutions:
- Practice wearing your mask during the day while watching TV or reading
- Use your machine’s ramp feature to start at lower pressure
- Try the “lights out” approach—put your mask on in darkness to reduce visual awareness
- Consider CPAP anxiety techniques
Getting used to CPAP therapy takes time for everyone, but stomach sleepers often need extra patience. Give yourself 2-3 weeks before concluding a mask doesn’t work.
CPAP Compliance and Your Insurance
Here’s something important to know: most insurance companies require proof of compliance to continue covering your CPAP supplies. CPAP compliance typically means using your machine at least 4 hours per night for 70% of nights in a 30-day period.
For stomach sleepers struggling with mask fit, this can create a vicious cycle: poor seal leads to therapy interruptions, which leads to non-compliance, which leads to insurance denying replacement supplies, which makes the problem worse.
If you’re having trouble meeting compliance requirements due to mask issues:
- Document your attempts and struggles
- Work with your sleep medicine provider to try different masks (many insurance plans cover mask exchanges within the first 30 days)
- Request a follow-up titration study if mask leaks are preventing effective therapy
- Consider out-of-pocket purchases for trial masks if insurance denies coverage
Don’t let compliance requirements prevent you from finding a mask that works. The goal is effective therapy, not just meeting an arbitrary usage threshold.
The Long-Term Health Picture
Let’s talk about why this matters beyond comfort. Untreated sleep apnea isn’t just about being tired—it dramatically increases your risks for:
- Cardiovascular disease: Sleep apnea increases heart disease and stroke risk by 2-3 times due to repeated oxygen desaturation and stress responses
- Metabolic dysfunction: The Connection between sleep apnea and diabetes is well-established, with OSA increasing insulin resistance
- Cognitive decline: CPAP therapy and brain fog are directly linked—untreated apnea accelerates cognitive aging
- Mental health: Strong correlation between sleep apnea and mental health, including depression and anxiety
Using your CPAP consistently—which requires a mask that actually works for your sleep position—can reduce these risks to near-baseline levels. CPAP therapy increases life expectancy when used correctly.
I share this not to scare you, but to emphasize that finding the right mask isn’t a luxury—it’s a medical necessity. If you’re a stomach sleeper, you deserve equipment that accommodates your sleep style rather than fighting against it.
Special Considerations for Stomach Sleepers
Traveling with CPAP
Stomach sleepers face unique challenges when traveling. Hotel pillows rarely accommodate CPAP masks well, and you can’t always pack your specialized CPAP pillow.
I recommend:
- Packing a travel CPAP machine and keeping a backup cushion in your travel kit
- Bringing a small wedge pillow or rolled towel to create mask clearance with standard hotel pillows
- Using masks with the most minimal design (P30i or DreamWear) for travel to maximize adaptability
Facial Hair Complications
Beards interfere with mask seals, and stomach sleeping compounds this problem by pressing facial hair into cushions.
CPAP masks for beards typically rely on nasal pillow designs that seal inside the nostril rather than on the skin. The P30i and similar nasal pillows bypass beard seal issues entirely.
If you have a full beard and sleep on your stomach, nasal pillows aren’t just recommended—they’re essentially mandatory for functional therapy.
Women-Specific Fit Issues
CPAP masks for women often need different sizing than unisex models. Women typically have smaller facial features, narrower nose bridges, and different facial contours.
Most of my recommended masks (P30i, N30i, DreamWear) come in multiple sizes including small options that work well for smaller facial structures. The F30i’s under-nose design is particularly good for women who find traditional full-face masks too large.
Children and Stomach Sleeping
Pediatric sleep apnea presents unique challenges. Kids are more likely to be stomach sleepers, but their facial structures change rapidly as they grow.
CPAP masks for children require special attention to fit and comfort. Nasal pillow options with minimal contact are often best for stomach-sleeping kids, but work closely with your pediatric sleep specialist.
Emerging Technology and Future Options
CPAP mask technology continues evolving. While I can’t test unreleased products, here are developments on the horizon that may benefit stomach sleepers:
Adhesive nasal masks: Some companies are developing stick-on nasal interfaces that eliminate headgear entirely. These could theoretically work well for stomach sleepers by removing pressure points.
Smart masks with position sensors: Integration of sleep position tracking with mask pressure adjustment could optimize therapy for stomach sleepers specifically.
Ultra-minimal pillow designs: Next-generation nasal pillows may use materials and engineering that reduce size even further while maintaining seal at higher pressures.
Alternatives to CPAP for Stomach Sleepers
If you’ve exhausted mask options and still can’t maintain effective therapy, other treatments exist:
Oral Appliances
Sleep apnea mouth guards (mandibular advancement devices) work by repositioning your jaw to keep airways open. They have no external components, making them ideal for stomach sleepers.
However, oral appliances are typically less effective than CPAP for moderate-to-severe sleep apnea. They work best for mild OSA or as an alternative when CPAP compliance fails despite good-faith efforts.
Surgical Options
Sleep apnea surgery includes several procedures from UPPP to hypoglossal nerve stimulation (Inspire therapy).
Surgery eliminates equipment entirely, which obviously solves stomach-sleeping compatibility issues. However, surgical success rates vary, and most procedures require significant recovery time.
Positional Therapy Devices
For position-dependent sleep apnea, devices that prevent back sleeping might be enough. But if you’re a stomach sleeper with apnea, positional therapy typically means training yourself OUT of stomach sleeping rather than into it.
BiPAP and ASV
BiPAP machines and ASV devices use different pressure delivery systems than standard CPAP. They work with the same masks, so they don’t inherently solve stomach-sleeping challenges, but the pressure changes can sometimes improve comfort.
Final Thoughts: Your Path Forward
Look, I’m not going to pretend stomach sleeping with CPAP is easy. It’s legitimately one of the hardest configurations in sleep apnea therapy. But thousands of people do it successfully every night, and the right equipment makes all the difference.
If I were advising you in person, here’s exactly what I’d recommend:
Start with the ResMed AirFit P30i. It’s the most universally successful mask for stomach sleepers I’ve encountered. If you’re not a mouth breather and don’t need extremely high pressures, this mask will probably work.
Get a proper CPAP pillow at the same time. Don’t try to make it work with a regular pillow—you’re setting yourself up for failure.
Give it two weeks minimum. The first few nights might be rough. Your brain needs time to stop perceiving the mask as a threat. Trust the process.
If the P30i doesn’t work, try the AirTouch N30i for a softer seal, or the DreamWear if ResMed’s fit doesn’t match your facial structure. If you mouth breathe, jump straight to the F30i.
Document everything. Keep notes on leak rates, AHI (apnea-hypopnea index), and comfort. This data helps your sleep medicine provider make informed adjustments and supports insurance claims if you need to try multiple masks.
The goal is effective therapy that you can sustain long-term. Stomach sleeping doesn’t have to prevent that—but it does require choosing equipment that works with your sleep style rather than against it.
Remember: the 16 hours you’re awake depend entirely on the quality of the 8 hours you sleep. Don’t settle for “good enough” equipment when your health is on the line. You deserve a CPAP setup that delivers restful, restorative sleep while accommodating the way you actually sleep.
Sweet dreams, stomach sleepers. You’ve got this.
Frequently Asked Questions
Q: Can I sleep on my stomach with a full-face CPAP mask?
A: Traditional full-face masks are extremely difficult for stomach sleeping due to their bulk. However, the ResMed AirFit F30i is specifically designed as a low-profile full-face option with top-of-head tubing that can work for stomach sleepers who must have mouth coverage. It’s still more challenging than nasal options, but it’s possible.
Q: Why does my mask leak more when I sleep on my stomach?
A: Pillow pressure pushes against your mask from multiple angles, breaking the seal between the cushion and your face. Top-of-head hose connections and minimal-contact designs (like nasal pillows) reduce this problem significantly.
Q: Will insurance cover multiple masks while I find one that works?
A: Most insurance plans allow mask exchanges within the first 30 days of purchase. Some provide a “trial period” specifically because mask fit is so personal. Check your specific plan’s durable medical equipment (DME) coverage.
Q: Can I switch between masks based on my sleep position?
A: Yes, many CPAP users keep multiple masks for different situations. However, I recommend finding one mask that works for all positions rather than switching nightly—consistency helps with therapy compliance.
Q: My sleep study showed I sleep on my side, but I wake up on my stomach. Which mask should I choose?
A: Choose based on where you end up, not where you start. If you’re waking on your stomach, you’re likely spending significant time there during the night. A mask that works for stomach sleeping will also work for side sleeping.
References
- Skarpsno ES, Mork PJ, Nilsen TIL, Holtermann A. Sleep positions and nocturnal body movements based on free-living accelerometer recordings: association with demographics, lifestyle, and insomnia symptoms. Nature and Science of Sleep. 2017;9:267-275. https://pubmed.ncbi.nlm.nih.gov/29138608/
- Weaver TE, Grunstein RR. Adherence to continuous positive airway pressure therapy: the challenge to effective treatment. Proceedings of the American Thoracic Society. 2008;5(2):173-178. https://pubmed.ncbi.nlm.nih.gov/18250209/
- Patel SR, White DP, Malhotra A, Stanchina ML, Ayas NT. Continuous positive airway pressure therapy for treating sleepiness in a diverse population with obstructive sleep apnea: results of a meta-analysis. Archives of Internal Medicine. 2003;163(5):565-571. https://pubmed.ncbi.nlm.nih.gov/12622603/
- Sawyer AM, Gooneratne NS, Marcus CL, Ofer D, Richards KC, Weaver TE. A systematic review of CPAP adherence across age groups: clinical and empiric insights for developing CPAP adherence interventions. Sleep Medicine Reviews. 2011;15(6):343-356. https://pubmed.ncbi.nlm.nih.gov/21652236/
- Bakker JP, Weaver TE, Parthasarathy S, Aloia MS. Adherence to CPAP: What should we be aiming for, and how can we get there? Chest. 2019;155(6):1272-1287. https://pubmed.ncbi.nlm.nih.gov/30597112/
- Martínez-García MA, Campos-Rodriguez F, Catalán-Serra P, et al. Cardiovascular mortality in obstructive sleep apnea in the elderly: role of long-term continuous positive airway pressure treatment: a prospective observational study. American Journal of Respiratory and Critical Care Medicine. 2012;186(9):909-916. https://pubmed.ncbi.nlm.nih.gov/22983957/
- Weaver TE, Maislin G, Dinges DF, et al. Relationship between hours of CPAP use and achieving normal levels of sleepiness and daily functioning. Sleep. 2007;30(6):711-719. https://pubmed.ncbi.nlm.nih.gov/17580592/
- Ravesloot MJ, White D, Heinzer R, Oksenberg A, Pépin JL. Efficacy of the new generation of devices for positional therapy for patients with positional obstructive sleep apnea: A systematic review of the literature and meta-analysis. Journal of Clinical Sleep Medicine. 2017;13(6):813-824. https://pubmed.ncbi.nlm.nih.gov/28454599/
- Rotenberg BW, Murariu D, Pang KP. Trends in CPAP adherence over twenty years of data collection: a flattened curve. Journal of Otolaryngology – Head & Neck Surgery. 2016;45(1):43. https://pubmed.ncbi.nlm.nih.gov/27473327/
- Epstein LJ, Kristo D, Strollo PJ Jr, et al. Clinical guideline for the evaluation, management and long-term care of obstructive sleep apnea in adults. Journal of Clinical Sleep Medicine. 2009;5(3):263-276. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2699173/
- Patil SP, Ayappa IA, Caples SM, Kimoff RJ, Patel SR, Harrod CG. Treatment of adult obstructive sleep apnea with positive airway pressure: an American Academy of Sleep Medicine systematic review, meta-analysis, and GRADE assessment. Journal of Clinical Sleep Medicine. 2019;15(2):301-334. https://pubmed.ncbi.nlm.nih.gov/30736888/
- Wozniak DR, Lasserson TJ, Smith I. Educational, supportive and behavioural interventions to improve usage of continuous positive airway pressure machines in adults with obstructive sleep apnoea. Cochrane Database of Systematic Reviews. 2014;(1):CD007736. https://pubmed.ncbi.nlm.nih.gov/24399660/
- Mehrtash M, Bakker JP, Ayas N. Predictors of continuous positive airway pressure adherence in patients with obstructive sleep apnea. Lung. 2019;197(2):115-121. https://pubmed.ncbi.nlm.nih.gov/30523424/
- Ravesloot MJ, van Maanen JP, Dun L, de Vries N. The undervalued potential of positional therapy in position-dependent snoring and obstructive sleep apnea-a review of the literature. Sleep and Breathing. 2013;17(1):39-49. https://pubmed.ncbi.nlm.nih.gov/22441662/
- Wickwire EM, Albrecht JS, Towe MM, et al. The impact of treatments for OSA on monetized health economic outcomes: a systematic review. Chest. 2019;155(5):947-961. https://pubmed.ncbi.nlm.nih.gov/30639340/
- Joosten SA, Hamilton GS, Naughton MT. Impact of weight loss management in OSA. Chest. 2017;152(1):194-203. https://pubmed.ncbi.nlm.nih.gov/28477954/
- Pépin JL, Bailly S, Tamisier R. Big Data in sleep apnoea: opportunities and challenges. Respirology. 2020;25(5):456-463. https://pubmed.ncbi.nlm.nih.gov/31943651/
- Kushida CA, Littner MR, Hirshkowitz M, et al. Practice parameters for the use of continuous and bilevel positive airway pressure devices to treat adult patients with sleep-related breathing disorders. Sleep. 2006;29(3):375-380. https://pubmed.ncbi.nlm.nih.gov/16553025/
For authoritative medical guidance on sleep apnea treatment, consult the American Academy of Sleep Medicine (aasm.org) or your healthcare provider.
⚠️ MEDICAL DISCLAIMER This blog provides general information only and is not a substitute for professional medical advice, diagnosis, or treatment. Sleep apnea is a serious condition, and CPAP equipment should be used under proper medical supervision. Always consult your doctor or sleep specialist before starting, stopping, or changing any therapy. I share personal experiences as a CPAP user, not as a medical professional. Individual results vary. For medical guidance, please consult a qualified clinician or the American Academy of Sleep Medicine (aasm.org).